Page 283 - Read Online
P. 283
Page 8 of 11 Conway et al. Vessel Plus 2020;4:25 I http://dx.doi.org/10.20517/2574-1209.2020.19
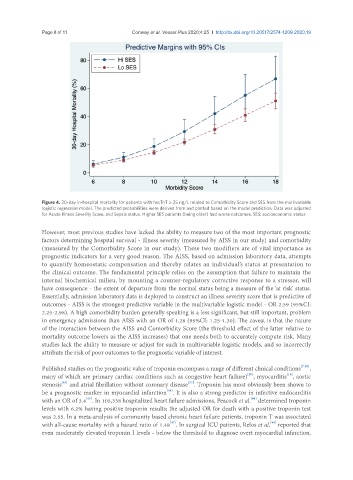
Figure 4. 30-day in-hospital mortality for patients with hscTnT ≥ 25 ng/L related to Comorbidity Score and SES from the multivariable
logistic regression model. The predicted probabilities were derived from and plotted based on the model prediction. Data was adjusted
for Acute Illness Severity Score, and Sepsis status. Higher SES patients (being older) had worse outcomes. SES: socioeconomic status
However, most previous studies have lacked the ability to measure two of the most important prognostic
factors determining hospital survival - illness severity (measured by AISS in our study) and comorbidity
(measured by the Comorbidity Score in our study). These two modifiers are of vital importance as
prognostic indicators for a very good reason. The AISS, based on admission laboratory data, attempts
to quantify homeostatic compensation and thereby relates an individual’s status at presentation to
the clinical outcome. The fundamental principle relies on the assumption that failure to maintain the
internal biochemical milieu, by mounting a counter-regulatory corrective response to a stressor, will
have consequence - the extent of departure from the normal status being a measure of the ‘at risk’ status.
Essentially, admission laboratory data is deployed to construct an illness severity score that is predictive of
outcomes - AISS is the strongest predictive variable in the multivariable logistic model - OR 2.59 (95%CI:
2.25-2.98). A high comorbidity burden generally speaking is a less significant, but still important, problem
in emergency admissions than AISS with an OR of 1.28 (95%CI: 1.25-1.30). The caveat is that the nature
of the interaction between the AISS and Comorbidity Score (the threshold effect of the latter relative to
mortality outcome lowers as the AISS increases) that one needs both to accurately compute risk. Many
studies lack the ability to measure or adjust for such in multivariable logistic models, and so incorrectly
attribute the risk of poor outcomes to the prognostic variable of interest.
Published studies on the prognostic value of troponin encompass a range of different clinical conditions [7-20] ,
[18]
[20]
many of which are primary cardiac conditions such as congestive heart failure) , myocarditis , aortic
[17]
[43]
stenosis and atrial fibrillation without coronary disease . Troponin has most obviously been shown to
be a prognostic marker in myocardial infarction . It is also a strong predictor in infective endocarditis
[44]
[45]
[46]
with an OR of 3.4 . In 105,338 hospitalized heart failure admissions, Peacock et al. determined troponin
levels with 6.2% having positive troponin results; the adjusted OR for death with a positive troponin test
was 2.55. In a meta-analysis of community based chronic heart failure patients, troponin T was associated
[48]
with all-cause mortality with a hazard ratio of 1.48 . In surgical ICU patients, Relos et al. reported that
[47]
even moderately elevated troponin I levels - below the threshold to diagnose overt myocardial infarction,