Page 107 - Read Online
P. 107
Page 4 of 13 Bradley et al. Plast Aesthet Res 2019;6:11 I http://dx.doi.org/10.20517/2347-9264.2019.06
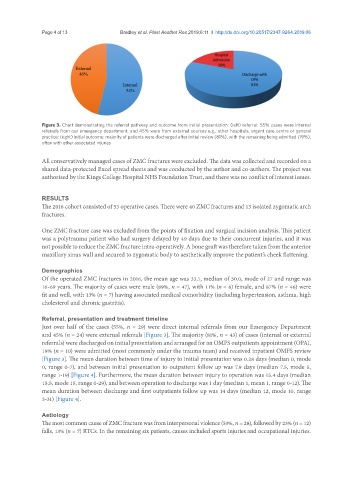
Figure 3. Chart demonstrating the referral pathway and outcome from initial presentation: (left) referral: 55% cases were internal
referrals from our emergency department, and 45% were from external sources e.g., other hospitals, urgent care centre or general
practice; (right) initial outcome: majority of patients were discharged after initial review (81%), with the remaining being admitted (19%),
often with other associated injuries
All conservatively managed cases of ZMC fractures were excluded. The data was collected and recorded on a
shared data-protected Excel spread sheets and was conducted by the author and co-authors. The project was
authorised by the Kings College Hospital NHS Foundation Trust, and there was no conflict of interest issues.
RESULTS
The 2016 cohort consisted of 53 operative cases. There were 40 ZMC fractures and 13 isolated zygomatic arch
fractures.
One ZMC fracture case was excluded from the points of fixation and surgical incision analysis. This patient
was a polytrauma patient who had surgery delayed by 49 days due to their concurrent injuries, and it was
not possible to reduce the ZMC fracture intra-operatively. A bone graft was therefore taken from the anterior
maxillary sinus wall and secured to zygomatic body to aesthetically improve the patient’s cheek flattening.
Demographics
Of the operated ZMC fractures in 2016, the mean age was 33.1, median of 30.0, mode of 27 and range was
16-69 years. The majority of cases were male (89%, n = 47), with 11% (n = 6) female, and 87% (n = 46) were
fit and well, with 13% (n = 7) having associated medical comorbidity (including hypertension, asthma, high
cholesterol and chronic gastritis).
Referral, presentation and treatment timeline
Just over half of the cases (55%, n = 29) were direct internal referrals from our Emergency Department
and 45% (n = 24) were external referrals [Figure 3]. The majority (81%, n = 43) of cases (internal or external
referrals) were discharged on initial presentation and arranged for an OMFS outpatients appointment (OPA),
19% (n = 10) were admitted (most commonly under the trauma team) and received inpatient OMFS review
[Figure 3]. The mean duration between time of injury to initial presentation was 0.28 days (median 0, mode
0, range 0-7), and between initial presentation to outpatient follow up was 7.9 days (median 7.5, mode 5,
range 1-19) [Figure 4]. Furthermore, the mean duration between injury to operation was 15.4 days (median
15.5, mode 15, range 0-29), and between operation to discharge was 1 day (median 1, mean 1, range 0-12). The
mean duration between discharge and first outpatients follow up was 14 days (median 12, mode 10, range
3-31) [Figure 4].
Aetiology
The most common cause of ZMC fracture was from interpersonal violence (53%, n = 28), followed by 23% (n = 12)
falls, 13% (n = 7) RTCs. In the remaining six patients, causes included sports injuries and occupational injuries.