Page 286 - Read Online
P. 286
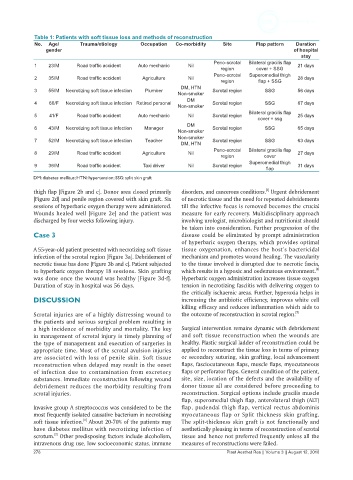
Table 1: Patients with soft tissue loss and methods of reconstruction
No. Age/ Trauma/etiology Occupation Co-morbidity Site Flap pattern Duration
gender of hospital
stay
Peno-scrotal Bilateral gracilis flap
1 23/M Road traffic accident Auto mechanic Nil 21 days
region cover + SSG
Peno-scrotal Superomedial thigh
2 35/M Road traffic accident Agriculture Nil 28 days
region flap + SSG
DM, HTN
3 55/M Necrotizing soft tissue infection Plumber Scrotal region SSG 56 days
Non-smoker
DM
4 60/F Necrotizing soft tissue infection Retired personal Scrotal region SSG 67 days
Non-smoker
Bilateral gracilis flap
5 41/F Road traffic accident Auto mechanic Nil Scrotal region 25 days
cover + ssg
DM
6 43/M Necrotizing soft tissue infection Manager Scrotal region SSG 65 days
Non-smoker
Non-smoker
7 52/M Necrotizing soft tissue infection Teacher Scrotal region SSG 63 days
DM, HTN
Peno-scrotal Bilateral gracilis flap
8 29/M Road traffic accident Agriculture Nil 27 days
region cover
Superomedial thigh
9 36/M Road traffic accident Taxi driver Nil Scrotal region 31 days
flap
DM: diabetes mellitus; HTN: hypertension; SSG: split skin graft
[3]
thigh flap [Figure 2b and c]. Donor area closed primarily disorders, and cancerous conditions. Urgent debridement
[Figure 2d] and penile region covered with skin graft. Six of necrotic tissue and the need for repeated debridements
sessions of hyperbaric oxygen therapy were administered. till the infective focus is removed becomes the crucial
Wounds healed well [Figure 2e] and the patient was measure for early recovery. Multidisciplinary approach
discharged by four weeks following injury. involving urologist, microbiologist and nutritionist should
be taken into consideration. Further progression of the
Case 3 disease could be eliminated by prompt administration
of hyperbaric oxygen therapy, which provides optimal
A 55-year-old patient presented with necrotizing soft tissue tissue oxygenation, enhances the host’s bactericidal
infection of the scrotal region [Figure 3a]. Debridement of mechanism and promotes wound healing. The vascularity
necrotic tissue has done [Figure 3b and c]. Patient subjected to the tissue involved is disrupted due to necrotic fascia,
to hyperbaric oxygen therapy 18 sessions. Skin grafting which results in a hypoxic and oedematous environment. [4]
was done once the wound was healthy [Figure 3d-f]. Hyperbaric oxygen administration increases tissue oxygen
Duration of stay in hospital was 56 days. tension in necrotizing fasciitis with delivering oxygen to
the critically ischaemic areas. Further, hyperoxia helps in
DISCUSSION increasing the antibiotic efficiency, improves white cell
killing efficacy and reduces inflammation which aids to
Scrotal injuries are of a highly distressing wound to the outcome of reconstruction in scrotal region. [5]
the patients and serious surgical problem resulting in
a high incidence of morbidity and mortality. The key Surgical intervention remains dynamic with debridement
in management of scrotal injury is timely planning of and soft tissue reconstruction when the wounds are
the type of management and execution of surgeries in healthy. Plastic surgical ladder of reconstruction could be
appropriate time. Most of the scrotal avulsion injuries applied to reconstruct the tissue loss in terms of primary
are associated with loss of penile skin. Soft tissue or secondary suturing, skin grafting, local advancement
reconstruction when delayed may result in the onset flaps, fasciocutaneous flaps, muscle flaps, myocutaneous
of infection due to contamination from excretory flaps or perforator flaps. General condition of the patient,
substances. Immediate reconstruction following wound site, size, location of the defects and the availability of
debridement reduces the morbidity resulting from donor tissue all are considered before proceeding to
scrotal injuries. reconstruction. Surgical options include gracilis muscle
flap, superomedial thigh flap, anterolateral thigh (ALT)
Invasive group A streptococcus was considered to be the flap, pudendal thigh flap, vertical rectus abdominis
most frequently isolated causative bacterium in necrotising myocutaneous flap or Split thickness skin grafting.
[1]
soft tissue infection. About 20-70% of the patients may The split-thickness skin graft is not functionally and
have diabetes mellitus with necrotizing infection of aesthetically pleasing in terms of reconstruction of scrotal
[2]
scrotum. Other predisposing factors include alcoholism, tissue and hence not preferred frequently unless all the
intravenous drug use, low socioeconomic status, immune measures of reconstructions were failed.
276 Plast Aesthet Res || Volume 3 || August 12, 2016