Page 261 - Read Online
P. 261
2
2
(median, 27 cm ; range, 4-250 cm ). The average number
of days to achieve wound closure was 39 days, with a
median of 21 days and a range of 3 to 236 days.
In general, patients tolerated NPWT with minimal
morbidity. One patient who had NPWT for fixation of
STSG developed cellulitis under the sponge secondary
to methicillin-resistant Staphylococcus aureus. The
cellulitis resolved after the discontinuation of the NPWT
and healed completely with no further interventions.
Seven patients developed maceration of the skin
under the wound VAC dressing, requiring temporary
discontinuation of NPWT.
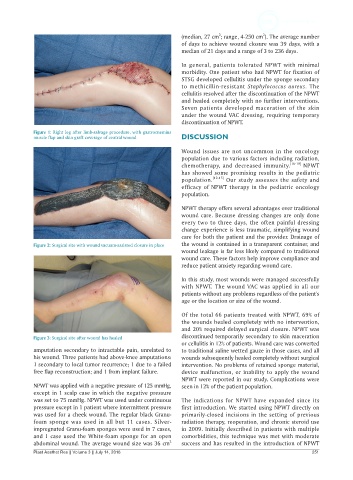
Figure 1: Right leg after limb-salvage procedure, with gastrocnemius
muscle flap and skin graft coverage of central wound DISCUSSION
Wound issues are not uncommon in the oncology
population due to various factors including radiation,
chemotherapy, and decreased immunity. [16-19] NPWT
has showed some promising results in the pediatric
population. [12-15] Our study assesses the safety and
efficacy of NPWT therapy in the pediatric oncology
population.
NPWT therapy offers several advantages over traditional
wound care. Because dressing changes are only done
every two to three days, the often painful dressing
change experience is less traumatic, simplifying wound
care for both the patient and the provider. Drainage of
Figure 2: Surgical site with wound vacuum-assisted closure in place the wound is contained in a transparent container, and
wound leakage is far less likely compared to traditional
wound care. These factors help improve compliance and
reduce patient anxiety regarding wound care.
In this study, most wounds were managed successfully
with NPWT. The wound VAC was applied in all our
patients without any problems regardless of the patient's
age or the location or size of the wound.
Of the total 66 patients treated with NPWT, 69% of
the wounds healed completely with no intervention,
and 20% required delayed surgical closure. NPWT was
Figure 3: Surgical site after wound has healed discontinued temporarily secondary to skin maceration
or cellulitis in 12% of patients. Wound care was converted
amputation secondary to intractable pain, unrelated to to traditional saline wetted gauze in those cases, and all
his wound. Three patients had above-knee amputations: wounds subsequently healed completely without surgical
1 secondary to local tumor recurrence; 1 due to a failed intervention. No problems of retained sponge material,
free flap reconstruction; and 1 from implant failure. device malfunction, or inability to apply the wound
NPWT were reported in our study. Complications were
NPWT was applied with a negative pressure of 125 mmHg, seen in 12% of the patient population.
except in 1 scalp case in which the negative pressure
was set to 75 mmHg. NPWT was used under continuous The indications for NPWT have expanded since its
pressure except in 1 patient where intermittent pressure first introduction. We started using NPWT directly on
was used for a cheek wound. The regular black Granu- primarily-closed incisions in the setting of previous
foam sponge was used in all but 11 cases. Silver- radiation therapy, reoperation, and chronic steroid use
impregnated Granu-foam sponges were used in 7 cases, in 2009. Initially described in patients with multiple
and 1 case used the White-foam sponge for an open comorbidities, this technique was met with moderate
2
abdominal wound. The average wound size was 36 cm success and has resulted in the introduction of NPWT
Plast Aesthet Res || Volume 3 || July 14, 2016 251