Page 81 - Read Online
P. 81
Page 8 of 11 Pang et al. Plast Aesthet Res 2021;8:49 https://dx.doi.org/10.20517/2347-9264.2021.42
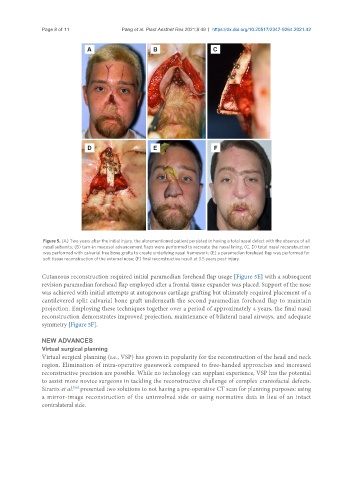
Figure 5. (A) Two years after the initial injury, the aforementioned patient persisted in having a total nasal defect with the absence of all
nasal subunits; (B) turn-in mucosal advancement flaps were performed to recreate the nasal lining; (C, D) total nasal reconstruction
was performed with calvarial free bone grafts to create underlying nasal framework; (E) a paramedian forehead flap was performed for
soft tissue reconstruction of the external nose; (F) final reconstructive result at 3.5 years post-injury.
Cutaneous reconstruction required initial paramedian forehead flap usage [Figure 5E] with a subsequent
revision paramedian forehead flap employed after a frontal tissue expander was placed. Support of the nose
was achieved with initial attempts at autogenous cartilage grafting but ultimately required placement of a
cantilevered split calvarial bone graft underneath the second paramedian forehead flap to maintain
projection. Employing these techniques together over a period of approximately 4 years, the final nasal
reconstruction demonstrates improved projection, maintenance of bilateral nasal airways, and adequate
symmetry [Figure 5F].
NEW ADVANCES
Virtual surgical planning
Virtual surgical planning (i.e., VSP) has grown in popularity for the reconstruction of the head and neck
region. Elimination of intra-operative guesswork compared to free-handed approaches and increased
reconstructive precision are possible. While no technology can supplant experience, VSP has the potential
to assist more novice surgeons in tackling the reconstructive challenge of complex craniofacial defects.
Stranix et al. presented two solutions to not having a pre-operative CT scan for planning purposes: using
[38]
a mirror-image reconstruction of the uninvolved side or using normative data in lieu of an intact
contralateral side.