Page 82 - Read Online
P. 82
Pandey et al. Plast Aesthet Res 2021;8:47 https://dx.doi.org/10.20517/2347-9264.2021.61 Page 5 of 12
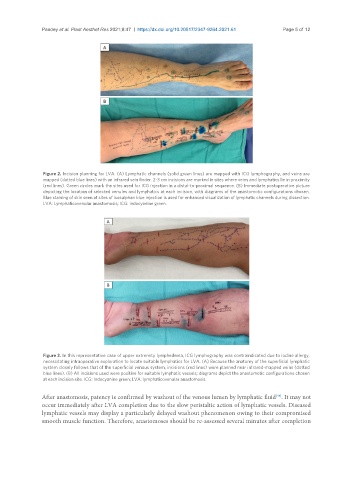
Figure 2. Incision planning for LVA. (A) Lymphatic channels (solid green lines) are mapped with ICG lymphography, and veins are
mapped (dotted blue lines) with an infrared vein finder. 2-3 cm incisions are marked in sites where veins and lymphatics lie in proximity
(red lines). Green circles mark the sites used for ICG injection in a distal-to-proximal sequence. (B) Immediate postoperative picture
depicting the location of selected venules and lymphatics at each incision, with diagrams of the anastomotic configurations chosen.
Blue staining of skin seen at sites of isosulphan blue injection is used for enhanced visualization of lymphatic channels during dissection.
LVA: Lymphaticovenular anastomosis; ICG: indocyanine green.
Figure 3. In this representative case of upper extremity lymphedema, ICG lymphography was contraindicated due to iodine allergy,
necessitating intraoperative exploration to locate suitable lymphatics for LVA. (A) Because the anatomy of the superficial lymphatic
system closely follows that of the superficial venous system, incisions (red lines) were planned near infrared-mapped veins (dotted
blue lines). (B) All incisions used were positive for suitable lymphatic vessels; diagrams depict the anastomotic configurations chosen
at each incision site. ICG: Indocyanine green; LVA: lymphaticovenular anastomosis.
[48]
After anastomosis, patency is confirmed by washout of the venous lumen by lymphatic fluid . It may not
occur immediately after LVA completion due to the slow peristaltic action of lymphatic vessels. Diseased
lymphatic vessels may display a particularly delayed washout phenomenon owing to their compromised
smooth muscle function. Therefore, anastomoses should be re-assessed several minutes after completion