Page 102 - Read Online
P. 102
Bonapace-Potvin et al. Plast Aesthet Res. 2025;12:34 https://dx.doi.org/10.20517/2347-9264.2025.65 Page 9 of 14
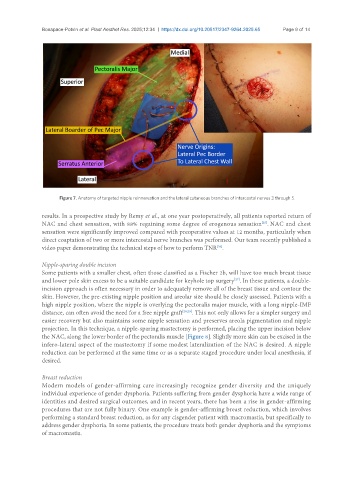
Figure 7. Anatomy of targeted nipple reinnervation and the lateral cutaneous branches of intercostal nerves 3 through 5.
results. In a prospective study by Remy et al., at one year postoperatively, all patients reported return of
NAC and chest sensation, with 88% regaining some degree of erogenous sensation . NAC and chest
[25]
sensation were significantly improved compared with preoperative values at 12 months, particularly when
direct coaptation of two or more intercostal nerve branches was performed. Our team recently published a
[26]
video paper demonstrating the technical steps of how to perform TNR .
Nipple-sparing double incision
Some patients with a smaller chest, often those classified as a Fischer 2b, will have too much breast tissue
and lower pole skin excess to be a suitable candidate for keyhole top surgery . In these patients, a double-
[27]
incision approach is often necessary in order to adequately remove all of the breast tissue and contour the
skin. However, the pre-existing nipple position and areolar size should be closely assessed. Patients with a
high nipple position, where the nipple is overlying the pectoralis major muscle, with a long nipple-IMF
distance, can often avoid the need for a free nipple graft [28,29] . This not only allows for a simpler surgery and
easier recovery but also maintains some nipple sensation and preserves areola pigmentation and nipple
projection. In this technique, a nipple-sparing mastectomy is performed, placing the upper incision below
the NAC, along the lower border of the pectoralis muscle [Figure 8]. Slightly more skin can be excised in the
infero-lateral aspect of the mastectomy if some modest lateralization of the NAC is desired. A nipple
reduction can be performed at the same time or as a separate staged procedure under local anesthesia, if
desired.
Breast reduction
Modern models of gender-affirming care increasingly recognize gender diversity and the uniquely
individual experience of gender dysphoria. Patients suffering from gender dysphoria have a wide range of
identities and desired surgical outcomes, and in recent years, there has been a rise in gender-affirming
procedures that are not fully binary. One example is gender-affirming breast reduction, which involves
performing a standard breast reduction, as for any cisgender patient with macromastia, but specifically to
address gender dysphoria. In some patients, the procedure treats both gender dysphoria and the symptoms
of macromastia.