Page 412 - Read Online
P. 412
Page 2 of 6 Paraskevas et al. Neuroimmunol Neuroinflammation 2018;5:49 I http://dx.doi.org/10.20517/2347-8659.2018.50
A B
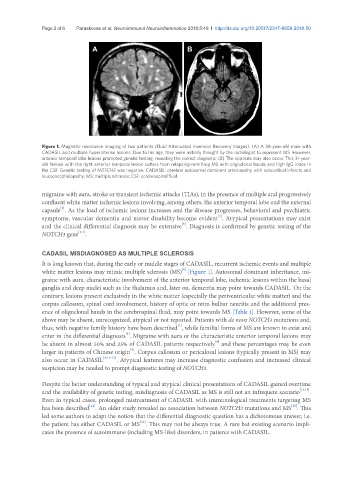
Figure 1. Magnetic resonance imaging of two patients (Fluid Attenuated Inversion Recovery images). (A) A 38-year-old male with
CADASIL and multiple hyperintense lesions. Due to his age, they were initially thought by the radiologist to represent MS. However,
anterior temporal lobe lesions prompted genetic testing, revealing the correct diagnosis; (B) The opposite may also occur. This 31-year-
old female with the right anterior temporal lesion suffers from relapsing-remitting MS with oligoclonal bands and high IgG index in
the CSF. Genetic testing of NOTCH3 was negative. CADASIL: cerebral autosomal dominant arteriopathy with subcortical infarcts and
leucoencephalopathy; MS: multiple sclerosis; CSF: cerebrospinal fluid
migraine with aura, stroke or transient ischemic attacks (TIAs), in the presence of multiple and progressively
confluent white matter ischemic lesions involving, among others, the anterior temporal lobe and the external
[3]
capsule . As the load of ischemic lesions increases and the disease progresses, behavioral and psychiatric
[4]
symptoms, vascular dementia and motor disability become evident . Atypical presentations may exist
[5]
and the clinical differential diagnosis may be extensive . Diagnosis is confirmed by genetic testing of the
[1,4]
NOTCH3 gene .
CADASIL MISDIAGNOSED AS MULTIPLE SCLEROSIS
It is long known that, during the early or middle stages of CADASIL, recurrent ischemic events and multiple
[6]
white matter lesions may mimic multiple sclerosis (MS) [Figure 1]. Autosomal dominant inheritance, mi-
graine with aura, characteristic involvement of the anterior temporal lobe, ischemic lesions within the basal
ganglia and deep nuclei such as the thalamus and, later on, dementia may point towards CADASIL. On the
contrary, lesions present exclusively in the white matter (especially the periventricular white matter) and the
corpus callosum, spinal cord involvement, history of optic or retro bulbar neuritis and the additional pres-
ence of oligoclonal bands in the cerebrospinal fluid, may point towards MS [Table 1]. However, some of the
above may be absent, unrecognized, atypical or not reported. Patients with de novo NOTCH3 mutations and,
[7]
thus, with negative family history have been described , while familial forms of MS are known to exist and
[5]
enter in the differential diagnosis . Migraine with aura or the characteristic anterior temporal lesions may
[8]
be absent in almost 50% and 25% of CADASIL patients respectively and these percentages may be even
[9]
larger in patients of Chinese origin . Corpus callosum or pericalosal lesions (typically present in MS) may
also occur in CADASIL [3,10-12] . Atypical features may increase diagnostic confusion and increased clinical
suspicion may be needed to prompt diagnostic testing of NOTCH3.
Despite the better understanding of typical and atypical clinical presentations of CADASIL gained overtime
and the availability of genetic testing, misdiagnosis of CADASIL as MS is still not an infrequent scenario [13,14] .
Even in typical cases, prolonged mistreatment of CADASIL with immunological treatments targeting MS
[15]
[14]
has been described . An older study revealed no association between NOTCH3 mutations and MS . This
led some authors to adapt the notion that the differential diagnostic question has a dichotomous answer, i.e.
[14]
the patient has either CADASIL or MS . This may not be always true. A rare but existing scenario impli-
cates the presence of autoimmune (including MS-like) disorders, in patients with CADASIL.