Page 91 - Read Online
P. 91
can present as generalized, focal, or complex partial MR spectroscopy of the basal ganglia and thalamus
seizures. Some cases may progress to status epilepticus may show a reduction of the N‑acetylaspartate/creatine
or nonconvulsive status epilepticus. Most of these cases (Cr) ratio in patients during involuntary movements. [30]
are refractory to treatment with standard antiepileptic
drugs but may respond well to immunosuppressive DIAGNOSTIC EVALUATIONS
drugs. One case report described nonconvulsive status
epilepticus lasting for 6 months that was refractory to The CSF profile in cases of anti‑NMDAR encephalitis
all immunomodulating therapies but showed marked typically shows pleocytosis and mild protein
[21]
improvement following removal of an ovarian tumor. elevations. The normal CSF profile does not exclude
Seizures in anti‑NMDAR encephalitic patients usually immune‑mediated disease. The brain MRI may be
[13]
have an extratemporal origin. [20,22] normal in up to 50% of cases. The EEG typically
shows diffuse slow or rhythmic activity. The EEG
The most commonly observed (90%) electroencephalogram of anti‑NMDAR encephalopathy is characterized
(EEG) pattern typically shows diffuse slowing or by an extreme delta brush, which can be found in
predominantly anterior slowing, but these phenomena up to 30% of cases. For specific antibody testing,
[23]
do not correlate with the clinical and MRI findings. it is recommended that both CSF and serum be
[13,16,23]
One‑third (34%) of patients exhibited focal assessed. In the majority of immune‑mediated limbic
slowing. One case series described a unique EEG encephalitis including anti‑NMDAR encephalitis, the
pattern of “extreme delta brush” in 30% of the patients CSF is more sensitive than the serum, excluding cases
in early stages of the disease. This pattern suggests the of VGKC‑complex autoantibody (Lgi1 and Caspr2),
occurrence of more severe disease (a more prolonged in which the serum may be more sensitive than
hospitalization). [23] the CSF. [13,31] The NMDAR‑IgG can be demonstrated
by the presence of immunologic reactivity to
Abnormal movement mouse brain tissue (especially in the hippocampus
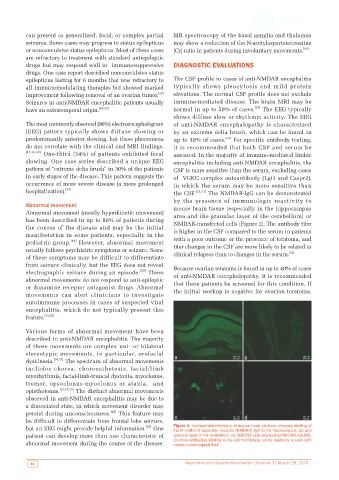
Abnormal movement (mostly hyperkinetic movement) area and the granular layer of the cerebellum) or
has been described in up to 80% of patients during
the course of the disease and may be the initial NMDAR‑transfected cells [Figure 2]. The antibody titer
is higher in the CSF compared to the serum in patients
manifestation in some patients, especially in the with a poor outcome or the presence of teratoma, and
pediatric group. [14] However, abnormal movement
usually follows psychiatric symptoms or seizure. Some titer changes in the CSF are more likely to be related to
[32]
of these symptoms may be difficult to differentiate clinical relapses than to changes in the serum.
from seizure clinically, but the EEG does not reveal Because ovarian teratoma is found in up to 40% of cases
electrographic seizure during an episode. [24] These of anti‑NMDAR encephalopathy, it is recommended
abnormal movements do not respond to anti‑epileptic
or dopamine receptor antagonist drugs. Abnormal that these patients be screened for this condition. If
movements can alert clinicians to investigate the initial workup is negative for ovarian teratoma,
autoimmune processes in cases of suspected viral
encephalitis, which do not typically present this
feature. [25,26]
Various forms of abnormal movement have been
described in anti‑NMDAR encephalitis. The majority
of these movements are complex uni‑ or bilateral
stereotypic movements, in particular, orofacial
dyskinesia. [14,27] The spectrum of abnormal movements
includes chorea, choreoathetosis, facial/limb
myorhythmia, facial‑limb‑truncal dystonia, myoclonus,
tremor, opsoclonus‑myoclonus or ataxia, and
opisthotonus. [14,27‑29] The distinct abnormal movements
observed in anti‑NMDAR encephalitis may be due to
a dissociated state, in which movement disorder may
[28]
persist during unconsciousness. This feature may
be difficult to differentiate from frontal lobe seizure,
[28]
but an EEG might provide helpful information. One Figure 2: Immunohistochemistry of mouse brain sections showing binding of
the N‑methyl‑D‑aspartate receptor (NMDAR)‑IgG to the hippocampus. (a) and
patient can develop more than one characteristic of granular layer of the cerebellum; (b) HEK293 cells expressing NMDAR (GluN1);
abnormal movement during the course of the disease. (c) show antibodies binding to the cell membrane; (d) no reactivity is seen with
normal cerebrospinal fluid
82 Neuroimmunol Neuroinflammation | Volume 3 | March 28, 2016