Page 196 - Read Online
P. 196
Page 8 of 11 Nakamura et al. Hepatoma Res 2019;5:16 I http://dx.doi.org/10.20517/2394-5079.2019.06
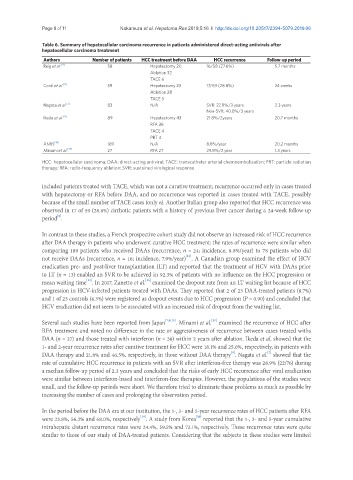
Table 6. Summary of hepatocellular carcinoma recurrence in patients administered direct-acting antivirals after
hepatocellular carcinoma treatment
Authors Number of patients HCC treatment before DAA HCC recurrence Follow-up period
Reig et al. [4] 58 Hepatectomy 20 16/58 (27.6%) 5.7 months
Ablation 32
TACE 6
Conti et al. [5] 59 Hepatectomy 23 17/59 (28.8%) 24 weeks
Ablation 28
TACE 5
Nagata et al. [7] 83 N/A SVR: 22.9%/3 years 2.3 years
Non-SVR: 40.0%/3 years
Ikeda et al. [9] 89 Hepatectomy 43 21.8%/2years 20.7 months
RFA 38
TACE 4
PRT 4
ANRS [10] 189 N/A 8.8%/year 20.2 months
Minami et al. [13] 27 RFA 27 29.8%/2 year 1.3 years
HCC: hepatocellular carcinoma; DAA: direct-acting antiviral; TACE: transcatheter arterial chemoembolization; PRT: particle radiation
therapy; RFA: radio-frequency ablation; SVR: sustained virological response
included patients treated with TACE, which was not a curative treatment; recurrence occurred only in cases treated
with hepatectomy or RFA before DAA, and no recurrence was reported in cases treated with TACE, possibly
because of the small number of TACE cases (only 6). Another Italian group also reported that HCC recurrence was
observed in 17 of 59 (28.8%) cirrhotic patients with a history of previous liver cancer during a 24-week follow-up
[5]
period .
In contrast to these studies, a French prospective cohort study did not observe an increased risk of HCC recurrence
after DAA therapy in patients who underwent curative HCC treatment: the rates of recurrence were similar when
comparing 189 patients who received DAAs (recurrence, n = 24; incidence, 8.8%/year) to 78 patients who did
[10]
not receive DAAs (recurrence, n = 16; incidence, 7.9%/year) . A Canadian group examined the effect of HCV
eradication pre- and post-liver transplantation (LT) and reported that the treatment of HCV with DAAs prior
to LT (n = 13) enabled an SVR to be achieved in 92.3% of patients with no influence on the HCC progression or
[14]
[15]
mean waiting time . In 2017, Zanetto et al. examined the dropout rate from an LT waiting list because of HCC
progression in HCV-infected patients treated with DAAs. They reported that 2 of 23 DAA-treated patients (8.7%)
and 1 of 23 controls (4.3%) were registered as dropout events due to HCC progression (P = 0.90) and concluded that
HCV eradication did not seem to be associated with an increased risk of dropout from the waiting list.
Several such studies have been reported from Japan [7,9,13] . Minami et al. examined the recurrence of HCC after
[13]
RFA treatment and noted no difference in the rate or aggressiveness of recurrence between cases treated withs
DAA (n = 27) and those treated with interferon (n = 38) within 2 years after ablation. Ikeda et al. showed that the
1- and 2-year recurrence rates after curative treatment for HCC were 18.1% and 25.0%, respectively, in patients with
DAA therapy and 21.8% and 46.5%, respectively, in those without DAA therapy . Nagata et al. showed that the
[7]
[9]
rate of cumulative HCC recurrence in patients with an SVR after interferon-free therapy was 28.9% (22/76) during
a median follow-up period of 2.3 years and concluded that the risks of early HCC recurrence after viral eradication
were similar between interferon-based and interferon-free therapies. However, the populations of the studies were
small, and the follow-up periods were short. We therefore tried to eliminate these problems as much as possible by
increasing the number of cases and prolonging the observation period.
In the period before the DAA era at our institution, the 1-, 3- and 5-year recurrence rates of HCC patients after RFA
were 23.8%, 56.2% and 68.0%, respectively . A study from Korea reported that the 1-, 3- and 5-year cumulative
[19]
[20]
intrahepatic distant recurrence rates were 24.4%, 59.5% and 73.1%, respectively. These recurrence rates were quite
similar to those of our study of DAA-treated patients. Considering that the subjects in these studies were limited