Page 335 - Read Online
P. 335
Lee et al. Liver resection in obese
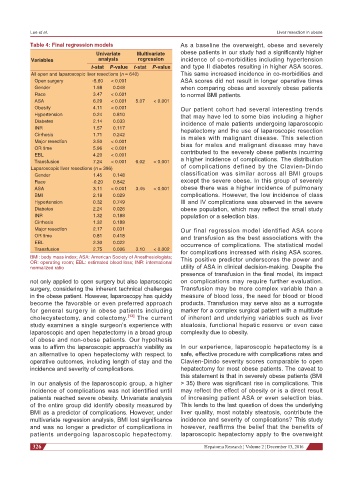
Table 4: Final regression models As a baseline the overweight, obese and severely
Univariate Multivariate obese patients in our study had a significantly higher
Variables analysis regression incidence of co-morbidities including hypertension
t-stat P-value t-stat P-value and type II diabetes resulting in higher ASA scores.
All open and laparoscopic liver resections (n = 640) This same increased incidence in co-morbidities and
Open surgery -5.60 < 0.001 ASA scores did not result in longer operative times
Gender 1.98 0.048 when comparing obese and severely obese patients
Race 3.47 < 0.001 to normal BMI patients.
ASA 6.29 < 0.001 5.07 < 0.001
Obesity 4.11 < 0.001 Our patient cohort had several interesting trends
Hypertension 0.24 0.810 that may have led to some bias including a higher
Diabetes 2.14 0.033 incidence of male patients undergoing laparoscopic
INR 1.57 0.117 hepatectomy and the use of laparoscopic resection
Cirrhosis 1.71 0.242 in males with malignant disease. This selection
Major resection 3.50 < 0.001 bias for males and malignant disease may have
OR time 5.96 < 0.001 contributed to the severely obese patients incurring
EBL 4.20 < 0.001
Transfusion 7.24 < 0.001 6.02 < 0.001 a higher incidence of complications. The distribution
Laparoscopic liver resections (n = 396) of complications defined by the Clavien-Dindo
Gender 1.45 0.148 classification was similar across all BMI groups
Race -0.20 0.842 except the severe obese. In this group of severely
ASA 3.11 < 0.001 3.45 < 0.001 obese there was a higher incidence of pulmonary
BMI 2.18 0.029 complications. However, the low incidence of class
Hypertension 0.32 0.749 III and IV complications was observed in the severe
Diabetes 2.24 0.026 obese population, which may reflect the small study
INR 1.32 0.188 population or a selection bias.
Cirrhosis 1.32 0.188
Major resection 2.17 0.031 Our final regression model identified ASA score
OR time 0.81 0.418 and transfusion as the best associations with the
EBL 2.30 0.022 occurrence of complications. The statistical model
Transfusion 2.75 0.006 3.10 < 0.002 for complications increased with rising ASA scores.
BMI: body mass index; ASA: American Society of Anesthesiologists; This positive predictor underscores the power and
OR: operating room; EBL: estimated blood loss; INR: international
normalized ratio utility of ASA in clinical decision-making. Despite the
presence of transfusion in the final model, its impact
not only applied to open surgery but also laparoscopic on complications may require further evaluation.
surgery, considering the inherent technical challenges Transfusion may be more complex variable than a
in the obese patient. However, laparoscopy has quickly measure of blood loss, the need for blood or blood
become the favorable or even preferred approach products. Transfusion may serve also as a surrogate
for general surgery in obese patients including marker for a complex surgical patient with a multitude
cholecystectomy, and colectomy. [13] The current of inherent and underlying variables such as liver
study examines a single surgeon’s experience with steatosis, functional hepatic reserve or even case
laparoscopic and open hepatectomy in a broad group complexity due to obesity.
of obese and non-obese patients. Our hypothesis
was to affirm the laparoscopic approach’s viability as In our experience, laparoscopic hepatectomy is a
an alternative to open hepatectomy with respect to safe, effective procedure with complications rates and
operative outcomes, including length of stay and the Clavien-Dindo severity scores comparable to open
incidence and severity of complications. hepatectomy for most obese patients. The caveat to
this statement is that in severely obese patients (BMI
In our analysis of the laparoscopic group, a higher > 35) there was significant rise in complications. This
incidence of complications was not identified until may reflect the effect of obesity or is a direct result
patients reached severe obesity. Univariate analysis of increasing patient ASA or even selection bias.
of the entire group did identify obesity measured by This lends to the last question of does the underlying
BMI as a predictor of complications. However, under liver quality, most notably steatosis, contribute the
multivariate regression analysis, BMI lost significance incidence and severity of complications? This study
and was no longer a predictor of complications in however, reaffirms the belief that the benefits of
patients undergoing laparoscopic hepatectomy. laparoscopic hepatectomy apply to the overweight
326 Hepatoma Research ¦ Volume 2 ¦ December 13, 2016