Page 54 - Read Online
P. 54
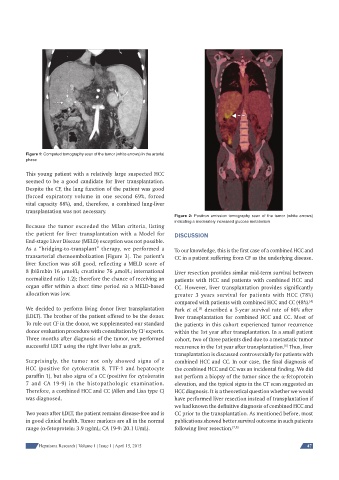
Figure 1: Computed tomography scan of the tumor (white arrows) in the arterial
phase
This young patient with a relatively large suspected HCC
seemed to be a good candidate for liver transplantation.
Despite the CF, the lung function of the patient was good
(forced expiratory volume in one second 69%, forced
vital capacity 88%), and, therefore, a combined lung-liver
transplantation was not necessary.
Figure 2: Positron emission tomography scan of the tumor (white arrows)
indicating a moderately increased glucose metabolism
Because the tumor exceeded the Milan criteria, listing
the patient for liver transplantation with a Model for DISCUSSION
End-stage Liver Disease (MELD) exception was not possible.
As a “bridging-to-transplant” therapy, we performed a To our knowledge, this is the first case of a combined HCC and
transarterial chemoembolization [Figure 3]. The patient’s CC in a patient suffering from CF as the underlying disease.
liver function was still good, reflecting a MELD score of
8 (bilirubin 16 mol/L; creatinine 76 mol/L; international Liver resection provides similar mid-term survival between
normalized ratio 1.2); therefore the chance of receiving an patients with HCC and patients with combined HCC and
organ offer within a short time period via a MELD-based CC. However, liver transplantation provides significantly
allocation was low. greater 3 years survival for patients with HCC (78%)
compared with patients with combined HCC and CC (48%).
[4 ]
We decided to perform living donor liver transplantation Park et al. described a 5-year survival rate of 60% after
[5]
(LDLT). The brother of the patient offered to be the donor. liver transplantation for combined HCC and CC. Most of
To rule out CF in the donor, we supplemented our standard the patients in this cohort experienced tumor recurrence
donor evaluation procedure with consultation by CF experts. within the 1st year after transplantation. In a small patient
Three months after diagnosis of the tumor, we performed cohort, two of three patients died due to a metastatic tumor
successful LDLT using the right liver lobe as graft. recurrence in the 1st year after transplantation. Thus, liver
[6]
transplantation is discussed controversially for patients with
Surprisingly, the tumor not only showed signs of a combined HCC and CC. In our case, the final diagnosis of
HCC (positive for cytokeratin 8, TTF-1 and hepatocyte the combined HCC and CC was an incidental finding. We did
paraffin 1), but also signs of a CC (positive for cytokeratin not perform a biopsy of the tumor since the -fetoprotein
7 and CA 19-9) in the histopathologic examination. elevation, and the typical signs in the CT scan suggested an
Therefore, a combined HCC and CC (Allen and Lisa type C) HCC diagnosis. It is a theoretical question whether we would
was diagnosed. have performed liver resection instead of transplantation if
we had known the definitive diagnosis of combined HCC and
Two years after LDLT, the patient remains disease-free and is CC prior to the transplantation. As mentioned before, most
in good clinical health. Tumor markers are all in the normal publications showed better survival outcome in such patients
range (-fetoprotein: 3.9 ng/mL; CA 19-9: 20.1 U/mL). following liver resection. [7,8]
Hepatoma Research | Volume 1 | Issue 1 | April 15, 2015 47