Page 112 - Read Online
P. 112
In order to achieve complete resolution of the disease,
surgery was offered. Pre-operative assessment showed that
the liver function was satisfactory for a major hepatectomy
(with a 6.6% indocyanine green retention rate at 15 min), and
there would be an adequate left-liver remnant. Laparotomy a b
was conducted in October 2012. The tumor was found to
have infiltrated to the right adrenal gland and the whole
length of the retrohepatic IVC. The left liver lobe had an
adequate volume and was free of tumor. The right lobe, c d
the caudate lobe of the liver, the right adrenal gland,
and the IVC were resected en bloc [Figure 2]. Immediate
reconstruction of the IVC was performed using a cadaveric
vein graft (5.5 cm long, 2.5 cm wide) [Figure 3]. The entire
operation lasted 10 h and the total IVC cross-clamping time e
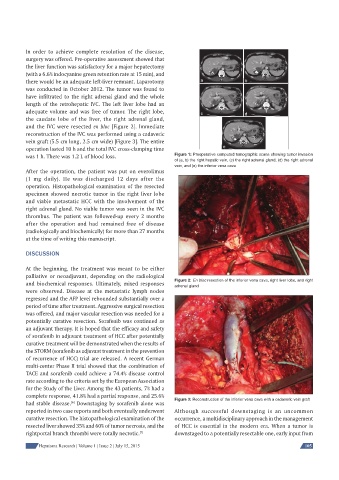
was 1 h. There was 1.2 L of blood loss. Figure 1: Preoperative computed tomographic scans showing tumor invasion
of (a, b) the right hepatic vein, (c) the right adrenal gland, (d) the right adrenal
vein, and (e) the inferior vena cava
After the operation, the patient was put on everolimus
(1 mg daily). He was discharged 12 days after the
operation. Histopathological examination of the resected
specimen showed necrotic tumor in the right liver lobe
and viable metastatic HCC with the involvement of the
right adrenal gland. No viable tumor was seen in the IVC
thrombus. The patient was followed-up every 2 months
after the operation and had remained free of disease
(radiologically and biochemically) for more than 27 months
at the time of writing this manuscript.
DISCUSSION
At the beginning, the treatment was meant to be either
palliative or neoadjuvant, depending on the radiological
and biochemical responses. Ultimately, mixed responses Figure 2: En bloc resection of the inferior vena cava, right liver lobe, and right
adrenal gland
were observed. Disease at the metastatic lymph nodes
regressed and the AFP level rebounded substantially over a
period of time after treatment. Aggressive surgical resection
was offered, and major vascular resection was needed for a
potentially curative resection. Sorafenib was continued as
an adjuvant therapy. It is hoped that the efficacy and safety
of sorafenib in adjuvant treatment of HCC after potentially
curative treatment will be demonstrated when the results of
the STORM (sorafenib as adjuvant treatment in the prevention
of recurrence of HCC) trial are released. A recent German
multi-center Phase II trial showed that the combination of
TACE and sorafenib could achieve a 74.4% disease control
rate according to the criteria set by the European Association
for the Study of the Liver. Among the 43 patients, 7% had a
complete response, 41.8% had a partial response, and 25.6%
had stable disease. Downstaging by sorafenib alone was Figure 3: Reconstruction of the inferior vena cava with a cadaveric vein graft
[6]
reported in two case reports and both eventually underwent Although successful downstaging is an uncommon
curative resection. The histopathological examination of the occurrence, a multidisciplinary approach in the management
resected liver showed 35% and 60% of tumor necrosis, and the of HCC is essential in the modern era. When a tumor is
rightportal branch thrombi were totally necrotic. [7] downstaged to a potentially resectable one, early input from
Hepatoma Research | Volume 1 | Issue 2 | July 15, 2015 105