Page 85 - Read Online
P. 85
Malerba et al. Hepatoma Res 2021;7:19 I http://dx.doi.org/10.20517/2394-5079.2020.131 Page 3 of 9
A B C
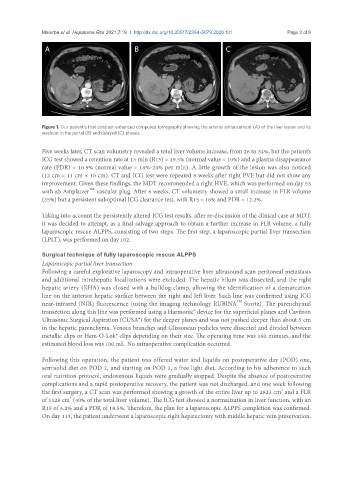
Figure 1. Our patient’s first contrast-enhanced computed tomography showing the arterial enhancement (A) of the liver lesion and its
washout in the portal (B) and delayed (C) phases.
Five weeks later, CT scan volumetry revealed a total liver volume increase, from 26 to 34%, but the patient’s
ICG test showed a retention rate at 15 min (R15) = 19.5% (normal value < 10%) and a plasma disappearance
rate (PDR) = 10.9% (normal value > 18%-24% per min). A little growth of the lesion was also noticed
(12 cm × 11 cm × 10 cm). CT and ICG test were repeated 8 weeks after right PVE but did not show any
improvement. Given these findings, the MDT recommended a right HVE, which was performed on day 53
TM
with ab Amplatzer vascular plug. After 6 weeks, CT volumetry showed a small increase in FLR volume
(35%) but a persistent suboptimal ICG clearance test, with R15 = 16% and PDR = 12.2%.
Taking into account the persistently altered ICG test results, after re-discussion of the clinical case at MDT,
it was decided to attempt, as a final salvage approach to obtain a further increase in FLR volume, a fully
laparoscopic rescue ALPPS, consisting of two steps. The first step, a laparoscopic partial liver transection
(LPLT), was performed on day 102.
Surgical technique of fully laparoscopic rescue ALPPS
Laparoscopic partial liver transection
Following a careful explorative laparoscopy and intraoperative liver ultrasound scan peritoneal metastasis
and additional intrahepatic localizations were excluded. The hepatic hilum was dissected, and the right
hepatic artery (RHA) was closed with a bulldog clamp, allowing the identification of a demarcation
line on the anterior hepatic surface between the right and left liver. Such line was confirmed using ICG
TM
near-infrared (NIR) fluorescence (using the imaging technology RUBINA Stortz). The parenchymal
transection along this line was performed using a Harmonic® device for the superficial planes and Cavitron
Ultrasonic Surgical Aspiration (CUSA®) for the deeper planes and was not pushed deeper than about 5 cm
in the hepatic parenchyma. Venous branches and Glissonean pedicles were dissected and divided between
metallic clips or Hem-O-Lok® clips depending on their size. The operating time was 160 minutes, and the
estimated blood loss was 100 mL. No intraoperative complication occurred.
Following this operation, the patient was offered water and liquids on postoperative day (POD) one,
semisolid diet on POD 2, and starting on POD 3, a free light diet. According to his adherence to such
oral nutrition protocol, endovenous liquids were gradually stopped. Despite the absence of postoperative
complications and a rapid postoperative recovery, the patient was not discharged, and one week following
3
the first surgery, a CT scan was performed showing a growth of the entire liver up to 2823 cm and a FLR
3
of 1128 cm (40% of the total liver volume). The ICG test showed a normalization in liver function, with an
R15 of 6.2% and a PDR of 18.5%. Therefore, the plan for a laparoscopic ALPPS completion was confirmed.
On day 113, the patient underwent a laparoscopic right hepatectomy with middle hepatic vein preservation.