Page 59 - Read Online
P. 59
Page 4 of 19 Lin et al. Cancer Drug Resist. 2026;9:14
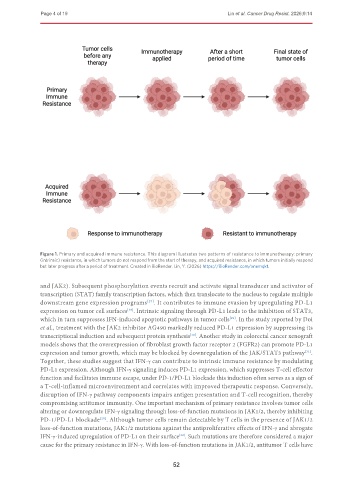
Figure 1. Primary and acquired immune resistance. This diagram illustrates two patterns of resistance to immunotherapy: primary
(intrinsic) resistance, in which tumors do not respond from the start of therapy, and acquired resistance, in which tumors initially respond
but later progress after a period of treatment. Created in BioRender. Lin, Y. (2026) https://BioRender.com/xnemqkt.
and JAK2). Subsequent phosphorylation events recruit and activate signal transducer and activator of
transcription (STAT) family transcription factors, which then translocate to the nucleus to regulate multiple
downstream gene expression programs . It contributes to immune evasion by upregulating PD-L1
[27]
expression on tumor cell surfaces . Intrinsic signaling through PD-L1 leads to the inhibition of STAT3,
[28]
which in turn suppresses IFN-induced apoptotic pathways in tumor cells . In the study reported by Doi
[29]
et al., treatment with the JAK2 inhibitor AG490 markedly reduced PD-L1 expression by suppressing its
transcriptional induction and subsequent protein synthesis . Another study in colorectal cancer xenograft
[30]
models shows that the overexpression of fibroblast growth factor receptor 2 (FGFR2) can promote PD-L1
expression and tumor growth, which may be blocked by downregulation of the JAK/STAT3 pathway .
[31]
Together, these studies suggest that IFN-γ can contribute to intrinsic immune resistance by modulating
PD-L1 expression. Although IFN-γ signaling induces PD-L1 expression, which suppresses T-cell effector
function and facilitates immune escape, under PD-1/PD-L1 blockade this induction often serves as a sign of
a T-cell-inflamed microenvironment and correlates with improved therapeutic response. Conversely,
disruption of IFN-γ pathway components impairs antigen presentation and T-cell recognition, thereby
compromising antitumor immunity. One important mechanism of primary resistance involves tumor cells
altering or downregulate IFN-γ signaling through loss-of-function mutations in JAK1/2, thereby inhibiting
PD-1/PD-L1 blockade . Although tumor cells remain detectable by T cells in the presence of JAK1/2
[20]
loss-of-function mutations, JAK1/2 mutations against the antiproliferative effects of IFN-γ and abrogate
IFN-γ-induced upregulation of PD-L1 on their surface . Such mutations are therefore considered a major
[32]
cause for the primary resistance in IFN-γ. With loss-of-function mutations in JAK1/2, antitumor T cells have
52