Page 347 - Read Online
P. 347
Page 6 of 11 Spieker et al. Vessel Plus 2020;4:29 I http://dx.doi.org/10.20517/2574-1209.2020.28
n n
P P
n n
P P
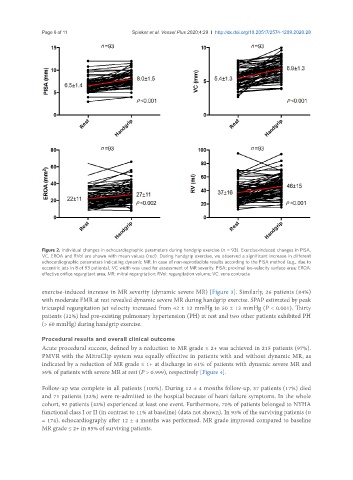
Figure 2. Individual changes in echocardiographic parameters during handgrip exercise (n = 93). Exercise-induced changes in PISA,
VC, EROA and RVol are shown with mean values (red). During handgrip exercise, we observed a significant increase in different
echocardiographic parameters indicating dynamic MR. In case of non-reproducible results according to the PISA method (e.g., due to
eccentric jets in 8 of 93 patients), VC width was used for assessment of MR severity. PISA: proximal iso-velocity surface area; EROA:
effective orifice regurgitant area; MR: mitral regurgitation; RVol: regurgitation volume; VC: vena contracta
exercise-induced increase in MR severity (dynamic severe MR) [Figure 3]. Similarly, 26 patients (84%)
with moderate FMR at rest revealed dynamic severe MR during handgrip exercise. SPAP estimated by peak
tricuspid regurgitation jet velocity increased from 42 ± 12 mmHg to 50 ± 13 mmHg (P < 0.001). Thirty
patients (32%) had pre-existing pulmonary hypertension (PH) at rest and two other patients exhibited PH
(> 60 mmHg) during handgrip exercise.
Procedural results and overall clinical outcome
Acute procedural success, defined by a reduction to MR grade ≤ 2+ was achieved in 215 patients (97%).
PMVR with the MitraClip system was equally effective in patients with and without dynamic MR, as
indicated by a reduction of MR grade ≤ 1+ at discharge in 61% of patients with dynamic severe MR and
59% of patients with severe MR at rest (P > 0.999), respectively [Figure 4].
Follow-up was complete in all patients (100%). During 12 ± 4 months follow-up, 37 patients (17%) died
and 71 patients (32%) were re-admitted to the hospital because of heart failure symptoms. In the whole
cohort, 92 patients (42%) experienced at least one event. Furthermore, 70% of patients belonged to NYHA
functional class I or II (in contrast to 11% at baseline) (data not shown). In 93% of the surviving patients (n
= 174), echocardiography after 12 ± 4 months was performed. MR grade improved compared to baseline
MR grade ≤ 2+ in 85% of surviving patients.