Page 46 - Read Online
P. 46
Page 10 of 13 Bencic et al. Plast Aesthet Res. 2025;12:30 https://dx.doi.org/10.20517/2347-9264.2025.38
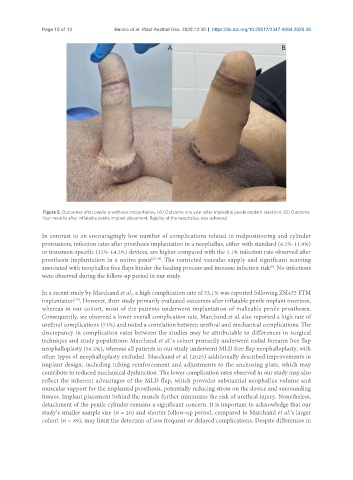
Figure 5. Outcomes after penile prosthesis implantation. (A) Outcome one year after malleable penile implant insertion; (B) Outcome
four months after inflatable penile implant placement. Rigidity of the neophallus was achieved.
In contrast to an encouragingly low number of complications related to malpositioning and cylinder
protrusions, infection rates after prosthesis implantation in a neophallus, either with standard (4.2%-11.9%)
or transmen-specific (12%-14.2%) devices, are higher compared with the 1.1% infection rate observed after
prosthesis implantation in a native penis [25-28] . The restricted vascular supply and significant scarring
associated with neophallus free flaps hinder the healing process and increase infection risk . No infections
[6]
were observed during the follow-up period in our study.
In a recent study by Marchand et al., a high complication rate of 53.1% was reported following ZSI475 FTM
[14]
implantation . However, their study primarily evaluated outcomes after inflatable penile implant insertion,
whereas in our cohort, most of the patients underwent implantation of malleable penile prostheses.
Consequently, we observed a lower overall complication rate. Marchand et al. also reported a high rate of
urethral complications (71%) and noted a correlation between urethral and mechanical complications. The
discrepancy in complication rates between the studies may be attributable to differences in surgical
technique and study populations: Marchand et al.’s cohort primarily underwent radial forearm free flap
neophalloplasty (56.2%), whereas all patients in our study underwent MLD free flap neophalloplasty, with
other types of neophalloplasty excluded. Marchand et al. (2025) additionally described improvements in
implant design, including tubing reinforcement and adjustments to the anchoring plate, which may
contribute to reduced mechanical dysfunction. The lower complication rates observed in our study may also
reflect the inherent advantages of the MLD flap, which provides substantial neophallus volume and
muscular support for the implanted prosthesis, potentially reducing stress on the device and surrounding
tissues. Implant placement behind the muscle further minimizes the risk of urethral injury. Nonetheless,
detachment of the penile cylinder remains a significant concern. It is important to acknowledge that our
study’s smaller sample size (n = 20) and shorter follow-up period, compared to Marchand et al.’s larger
cohort (n = 89), may limit the detection of less frequent or delayed complications. Despite differences in