Page 45 - Read Online
P. 45
Bencic et al. Plast Aesthet Res. 2025;12:30 https://dx.doi.org/10.20517/2347-9264.2025.38 Page 9 of 13
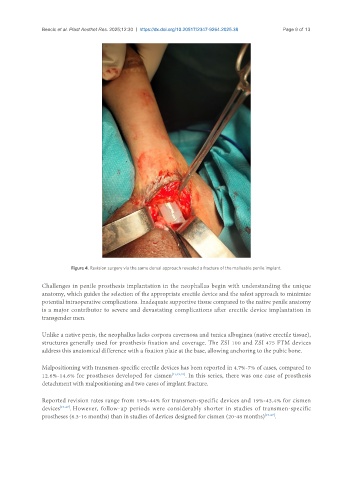
Figure 4. Revision surgery via the same dorsal approach revealed a fracture of the malleable penile implant.
Challenges in penile prosthesis implantation in the neophallus begin with understanding the unique
anatomy, which guides the selection of the appropriate erectile device and the safest approach to minimize
potential intraoperative complications. Inadequate supportive tissue compared to the native penile anatomy
is a major contributor to severe and devastating complications after erectile device implantation in
transgender men.
Unlike a native penis, the neophallus lacks corpora cavernosa and tunica albuginea (native erectile tissue),
structures generally used for prosthesis fixation and coverage. The ZSI 100 and ZSI 475 FTM devices
address this anatomical difference with a fixation plate at the base, allowing anchoring to the pubic bone.
Malpositioning with transmen-specific erectile devices has been reported in 4.7%-7% of cases, compared to
12.6%-14.6% for prostheses developed for cismen [17,19,22] . In this series, there was one case of prosthesis
detachment with malpositioning and two cases of implant fracture.
Reported revision rates range from 19%-44% for transmen-specific devices and 19%-43.4% for cismen
devices [17-27] . However, follow-up periods were considerably shorter in studies of transmen-specific
prostheses (6.3-16 months) than in studies of devices designed for cismen (20-48 months) [17-27] .