Page 226 - Read Online
P. 226
Chen et al. Neuroimmunol Neuroinflammation 2018;5:31 I http://dx.doi.org/10.20517/2347-8659.2018.23 Page 3 of 7
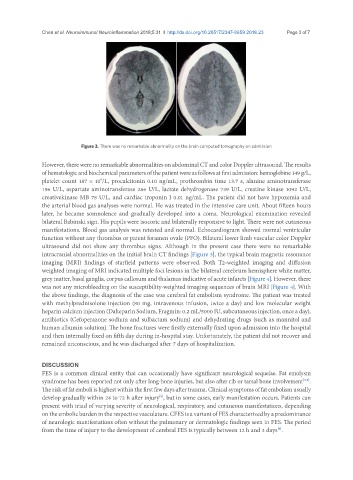
Figure 3. There was no remarkable abnormality on the brain computed tomography on admission
However, there were no remarkable abnormalities on abdominal CT and color Doppler ultrasound. The results
of hematologic and biochemical parameters of the patient were as follows at first admission: hemoglobine 149 g/L,
platelet count 187 × 10 /L, procalcitonin 0.10 ng/mL, prothrombin time 13.7 s, alanine aminotransferase
9
196 U/L, aspartate aminotransferase 286 U/L, lactate dehydrogenase 739 U/L, creatine kinase 1092 U/L,
creativekinase MB 78 U/L, and cardiac troponin I 0.01 ng/mL. The patient did not have hypoxemia and
the arterial blood gas analyses were normal. He was treated in the intensive care unit. About fifteen hours
later, he became somnolence and gradually developed into a coma. Neurological examination revealed
bilateral Babinski sign. His pupils were isocoric and bilaterally responsive to light. There were not cutaneous
manifestations. Blood gas analysis was retested and normal. Echocardiogram showed normal ventricular
function without any thrombus or patent foramen ovale (PFO). Bilateral lower limb vascular color Doppler
ultrasound did not show any thrombus signs. Although in the present case there were no remarkable
intracranial abnormalities on the initial brain CT findings [Figure 3], the typical brain magnetic resonance
imaging (MRI) findings of starfield patterns were observed. Both T2-weighted imaging and diffusion
weighted imaging of MRI indicated multiple foci lesions in the bilateral cerebrum hemisphere white matter,
grey matter, basal ganglia, corpus callosum and thalamus indicative of acute infarcts [Figure 4]. However, there
was not any microbleeding on the susceptibility-weighted imaging sequences of brain MRI [Figure 4]. With
the above findings, the diagnosis of the case was cerebral fat embolism syndrome. The patient was treated
with methylprednisolone injection (80 mg, intravenous infusion, twice a day) and low molecular weight
heparin calcium injection (Dalteparin Sodium, Fragmin: 0.2 mL/5000 IU, subcutaneous injection, once a day),
antibiotics (Cefoperazone sodium and sulbactam sodium) and dehydrating drugs (such as mannitol and
human albumin solution). The bone fractures were firstly externally fixed upon admission into the hospital
and then internally fixed on fifth day during in-hospital stay. Unfortunately, the patient did not recover and
remained unconscious, and he was discharged after 7 days of hospitalization.
DISCUSSION
FES is a common clinical entity that can occasionally have significant neurological sequelae. Fat emolysm
syndrome has been reported not only after long-bone injuries, but also after rib or tarsal bone involvement .
[3,4]
The risk of fat emboli is highest within the first few days after trauma. Clinical symptoms of fat embolism usually
[5]
develop gradually within 24 to 72 h after injury , but in some cases, early manifestation occurs. Patients can
present with triad of varying severity of neurological, respiratory, and cutaneous manifestations, depending
on the embolic burden in the respective vasculature. CFES is a variant of FES characterized by a predominance
of neurologic manifestations often without the pulmonary or dermatologic findings seen in FES. The period
from the time of injury to the development of cerebral FES is typically between 12 h and 3 days .
[6]