Page 908 - Read Online
P. 908
Park et al. Mini-invasive Surg 2020;4:87 I http://dx.doi.org/10.20517/2574-1225.2020.87 Page 7 of 16
P I 2
P
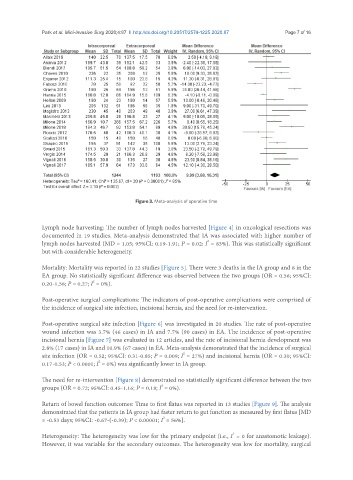
Figure 3. Meta-analysis of operative time
Lymph node harvesting: The number of lymph nodes harvested [Figure 4] in oncological resections was
documented in 19 studies. Meta-analysis demonstrated that IA was associated with higher number of
2
lymph nodes harvested (MD = 1.05; 95%CI: 0.19-1.91; P = 0.02; I = 83%). This was statistically significant
but with considerable heterogeneity.
Mortality: Mortality was reported in 22 studies [Figure 5]. There were 3 deaths in the IA group and 8 in the
EA group. No statistically significant difference was observed between the two groups (OR = 0.56; 95%CI:
2
0.20-1.58; P = 0.27; I = 0%).
Post-operative surgical complications: The indicators of post-operative complications were comprised of
the incidence of surgical site infection, incisional hernia, and the need for re-intervention.
Post-operative surgical site infection [Figure 6] was investigated in 20 studies. The rate of post-operative
wound infection was 3.7% (46 cases) in IA and 7.7% (90 cases) in EA. The incidence of post-operative
incisional hernia [Figure 7] was evaluated in 12 articles, and the rate of incisional hernia development was
2.8% (17 cases) in IA and 10.9% (67 cases) in EA. Meta-analysis demonstrated that the incidence of surgical
2
site infection (OR = 0.52; 95%CI: 0.31-0.85; P = 0.009; I = 27%) and incisional hernia (OR = 0.30; 95%CI:
2
0.17-0.53; P < 0.0001; I = 0%) was significantly lower in IA group.
The need for re-intervention [Figure 8] demonstrated no statistically significant difference between the two
2
groups (OR = 0.72; 95%CI: 0.45-1.16; P = 0.18; I = 0%).
Return of bowel function outcomes: Time to first flatus was reported in 13 studies [Figure 9]. The analysis
demonstrated that the patients in IA group had faster return to gut function as measured by first flatus [MD
2
= -0.53 days; 95%CI: -0.67-(-0.39); P < 0.00001; I = 56%].
2
Heterogeneity: The heterogeneity was low for the primary endpoint (i.e., I = 0 for anastomotic leakage).
However, it was variable for the secondary outcomes. The heterogeneity was low for mortality, surgical