Page 736 - Read Online
P. 736
Palacios Mini-invasive Surg 2020;4:73 I http://dx.doi.org/10.20517/2574-1225.2020.72 Page 5 of 24
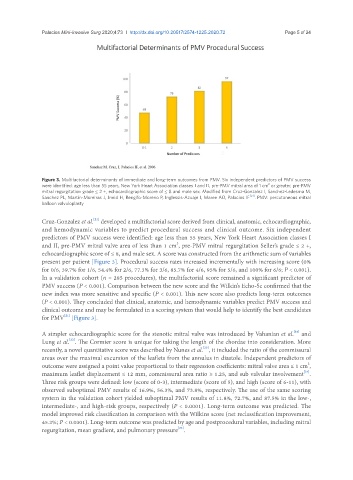
Figure 3. Multifactorial determinants of immediate and long-term outcomes from PMV. Six independent predictors of PMV success
2
were identified: age less than 55 years, New York Heart Association classes I and II, pre-PMV mitral area of 1 cm or greater, pre-PMV
mitral regurgitation grade ≤ 2 +, echocardiographic score of ≤ 8 and male sex. Modified from Cruz-Gonzalez I, Sanchez-Ledesma M,
Sanchez PL, Martin-Moreiras J, Jneid H, Rengifo-Moreno P, Inglessis-Azuaje I, Maree AO, Palacios IF [21] . PMV: percutaneous mitral
balloon valvuloplasty
[21]
Cruz-Gonzalez et al. developed a multifactorial score derived from clinical, anatomic, echocardiographic,
and hemodynamic variables to predict procedural success and clinical outcome. Six independent
predictors of PMV success were identified: age less than 55 years, New York Heart Association classes I
2
and II, pre-PMV mitral valve area of less than 1 cm , pre-PMV mitral regurgitation Seller’s grade ≤ 2 +,
echocardiographic score of ≤ 8, and male sex. A score was constructed from the arithmetic sum of variables
present per patient [Figure 3]. Procedural success rates increased incrementally with increasing score (0%
for 0/6, 39.7% for 1/6, 54.4% for 2/6, 77.3% for 3/6, 85.7% for 4/6, 95% for 5/6, and 100% for 6/6; P < 0.001).
In a validation cohort (n = 285 procedures), the multifactorial score remained a significant predictor of
PMV success (P < 0.001). Comparison between the new score and the Wilkin’s Echo-Sc confirmed that the
new index was more sensitive and specific (P < 0.001). This new score also predicts long-term outcomes
(P < 0.001). They concluded that clinical, anatomic, and hemodynamic variables predict PMV success and
clinical outcome and may be formulated in a scoring system that would help to identify the best candidates
for PMV [Figure 3].
[21]
A simpler echocardiographic score for the stenotic mitral valve was introduced by Vahanian et al. and
[16]
[22]
Lung et al. . The Cormier score is unique for taking the length of the chordae into consideration. More
recently, a novel quantitative score was described by Nunes et al. , it included the ratio of the commissural
[23]
areas over the maximal excursion of the leaflets from the annulus in diastole. Independent predictors of
outcome were assigned a point value proportional to their regression coefficients: mitral valve area ≤ 1 cm ,
2
[24]
maximum leaflet displacement ≤ 12 mm, commissural area ratio ≥ 1.25, and sub valvular involvement .
Three risk groups were defined: low (score of 0-3), intermediate (score of 5), and high (score of 6-11), with
observed suboptimal PMV results of 16.9%, 56.3%, and 73.8%, respectively. The use of the same scoring
system in the validation cohort yielded suboptimal PMV results of 11.8%, 72.7%, and 87.5% in the low-,
intermediate-, and high-risk groups, respectively (P < 0.0001). Long-term outcome was predicted. The
model improved risk classification in comparison with the Wilkins score (net reclassification improvement,
45.2%; P < 0.0001). Long-term outcome was predicted by age and postprocedural variables, including mitral
regurgitation, mean gradient, and pulmonary pressure .
[23]