Page 198 - Read Online
P. 198
Cicero et al. Mini-invasive Surg 2019;3:25 I http://dx.doi.org/10.20517/2574-1225.2018.012 Page 5 of 11
A B
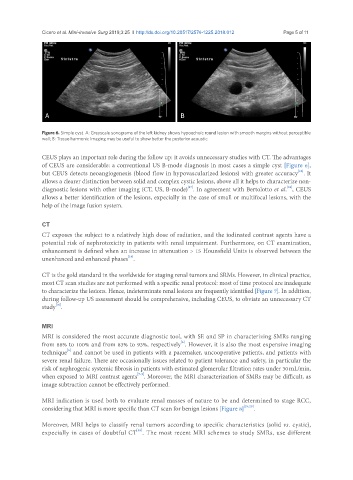
Figure 6. Simple cyst. A: Greyscale sonograms of the left kidney shows hypoechoic round lesion with smooth margins without perceptible
wall; B: Tissue harmonic imaging may be useful to show better the posterior acoustic
CEUS plays an important role during the follow up: it avoids unnecessary studies with CT. The advantages
of CEUS are considerable: a conventional US B-mode diagnosis in most cases a simple cyst [Figure 6],
[16]
but CEUS detects neoangiogenesis (blood flow in hypovascularized lesions) with greater accuracy . It
allows a clearer distinction between solid and complex cystic lesions, above all it helps to characterize non-
[17]
[18]
diagnostic lesions with other imaging (CT, US, B-mode) . In agreement with Bertolotto et al. , CEUS
allows a better identification of the lesions, expecially in the case of small or multifocal lesions, with the
help of the image fusion system.
CT
CT exposes the subject to a relatively high dose of radiation, and the iodinated contrast agents have a
potential risk of nephrotoxicity in patients with renal impairment. Furthermore, on CT examination,
enhancement is defined when an increase in attenuation > 15 Hounsfield Units is observed between the
[19]
unenhanced and enhanced phases .
CT is the gold standard in the worldwide for staging renal tumors and SRMs. However, in clinical practice,
most CT scan studies are not performed with a specific renal protocol: most of time protocol are inadequate
to characterize the lesions. Hence, indeterminate renal lesions are frequently identified [Figure 7]. In addition,
during follow-up US assessment should be comprehensive, including CEUS, to obviate an unnecessary CT
[16]
study .
MRI
MRI is considered the most accurate diagnostic tool, with SE and SP in characterizing SMRs ranging
[6]
from 88% to 100% and from 83% to 93%, respectively . However, it is also the most expensive imaging
[6]
technique and cannot be used in patients with a pacemaker, uncooperative patients, and patients with
severe renal failure. There are occasionally issues related to patient tolerance and safety, in particular the
risk of nephrogenic systemic fibrosis in patients with estimated glomerular filtration rates under 30 mL/min,
[7-9]
when exposed to MRI contrast agents . Moreover, the MRI characterization of SMRs may be difficult, as
image subtraction cannot be effectively performed.
MRI indication is used both to evaluate renal masses of nature to be and determined to stage RCC,
considering that MRI is more specific than CT scan for benign lesions [Figure 8] [19,20] .
Moreover, MRI helps to classify renal tumors according to specific characteristics (solid vs. cystic),
[18]
expecially in cases of doubtful CT . The most recent MRI schemes to study SMRs, use different