Page 147 - Read Online
P. 147
de Pascale et al. Mini-invasive Surg 2019;3:18 I http://dx.doi.org/10.20517/2574-1225.2019.04 Page 5 of 10
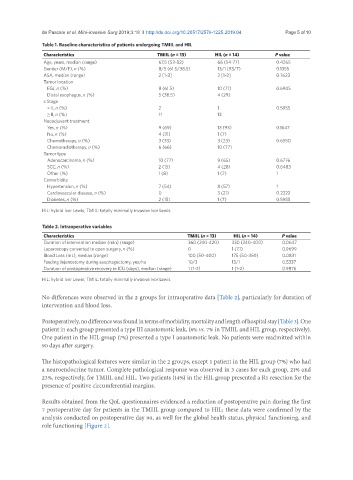
Table 1. Baseline characteristics of patients undergoing TMIIL and HIL
Characteristics TMIIL (n = 13) HIL (n = 14) P value
Age, years, median (range) 67.5 (53-82) 66 (54-77) 0.4265
Gender (M/F), n (%) 8/5 (61.5/38.5) 13/1 (93/7) 0.1355
ASA, median (range) 2 [1-3] 2 [1-3] 0.7623
Tumor location
EGJ, n (%) 8 (61.5) 10 (71) 0.6945
Distal esophagus, n (%) 5 (38.5) 4 (29)
c Stage
< II, n (%) 2 1 0.5955
≥ II, n (%) 11 13
Neoadjuvant treatment
Yes, n (%) 9 (69) 13 (93) 0.1647
No, n (%) 4 (31) 1 (7)
Chemotherapy, n (%) 3 (33) 3 (23) 0.6550
Chemoradiotherapy, n (%) 6 (66) 10 (77)
Tumor type
Adenocarcinoma, n (%) 10 (77) 9 (65) 0.6776
SCC, n (%) 2 (15) 4 (28) 0.6483
Other (%) 1 (8) 1 (7) 1
Comorbidity
Hypertension, n (%) 7 (54) 8 (57) 1
Cardiovascular disease, n (%) 0 3 (21) 0.2222
Diabetes, n (%) 2 (15) 1 (7) 0.5955
HIL: hybrid Ivor Lewis; TMIIL: totally minimally invasive Ivor Lewis
Table 2. Intraoperative variables
Characteristics TMIIL (n = 13) HIL (n = 14) P value
Duration of intervention median (min) (range) 360 (240-420) 330 (240-400) 0.0647
Laparoscopy converted to open surgery, n (%) 0 1 (7.1) 0.9699
Blood Loss (mL), median (range) 100 (50-400) 175 (50-350) 0.0831
Feeding Jejunostomy during esophagectomy, yes/no 10/3 13/1 0.5337
Duration of postoperative recovery in ICU (days), median (range) 1 (1-2) 1 (1-2) 0.9876
HIL: hybrid Ivor Lewis; TMIIL: totally minimally invasive Ivor Lewis
No differences were observed in the 2 groups for intraoperative data [Table 2], particularly for duration of
intervention and blood loss.
Postoperatively, no difference was found in terms of morbidity, mortality and length of hospital stay [Table 3]. One
patient in each group presented a type III anastomotic leak, (8% vs. 7% in TMIIL and HIL group, respectively).
One patient in the HIL group (7%) presented a type I anastomotic leak. No patients were readmitted within
90 days after surgery.
The histopathological features were similar in the 2 groups, except 1 patient in the HIL group (7%) who had
a neuroendocrine tumor. Complete pathological response was observed in 3 cases for each group, 21% and
23%, respectively, for TMIIL and HIL. Two patients (14%) in the HIL group presented a R1 resection for the
presence of positive circumferential margins.
Results obtained from the QoL questionnaires evidenced a reduction of postoperative pain during the first
7 postoperative day for patients in the TMIIL group compared to HIL; these data were confirmed by the
analysis conducted on postoperative day 90, as well for the global health status, physical functioning, and
role functioning [Figure 2].