Page 158 - Read Online
P. 158
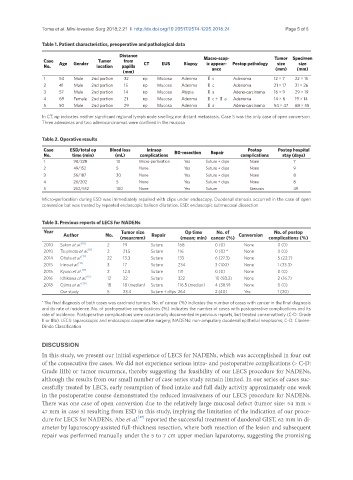
Toma et al. Mini-invasive Surg 2018;2:21 I http://dx.doi.org/10.20517/2574-1225.2018.24 Page 5 of 8
Table 1. Patient characteristics, preoperative and pathological data
Distance Macro-scop- Tumor Specimen
Case Age Gender Tumor from CT EUS Biopsy ic appear- Postop pathology size size
No. location papilla ance (mm) (mm)
(mm)
1 54 Male 2nd portion 32 np Mucosa Adenma Ⅱ c Adenoma 12 × 7 22 × 15
2 41 Male 2nd portion 15 np Mucosa Adenma Ⅱ c Adenoma 21 × 17 31 × 26
3 57 Male 2nd portion 14 np Mucosa Atypia Ⅱ a Adeno-carcinoma 16 × 9 29 × 19
4 69 Female 2nd portion 21 np Mucosa Adenma Ⅱ c + Ⅱ a Adenoma 14 × 6 19 × 14
5 50 Male 2nd portion 29 np Mucosa Adenma Ⅱ a Adeno-carcinoma 54 × 47 68 × 55
In CT, np indicates neither significant regional lymph node swelling nor distant metastasis. Case 5 was the only case of open conversion.
Three adenomas and two adenocarcinomas were confined in the mucosa
Table 2. Operative results
Case ESD/total op Blood loss Intraop Postop Postop hospital
No. time (min) (mL) complications R0-resection Repair complications stay (days)
1 98/228 10 Micro-perforation Yes Suture + clips None 7
2 49/152 5 None Yes Suture + clips None 9
3 56/187 30 None Yes Suture + clips None 8
4 26/202 5 None Yes Suture + clips None 8
5 252/552 100 None Yes Suture Stenosis 49
Micro-perforation during ESD was immediately repaired with clips under endoscopy. Duodenal stenosis occurred in the case of open
conversion but was treated by repeated endoscopic balloon dilatation. ESD: endoscopic submucosal dissection
Table 3. Previous reports of LECS for NADENs
Year Tumor size Op time No. of No. of postop
Author No. Repair Conversion
(mean:mm) (mean; min) cancer (%) complications (%)
2010 Sakon et al. [10] 2 19 Suture 168 0 (0) None 0 (0)
[11]
2010 Tsujimoto et al. 2 21.5 Suture 116 0 (0) * None 0 (0)
[12]
2014 Ohata et al. 22 13.3 Suture 133 6 (27.3) None 5 (22.7)
[13]
2015 Irino et al. 3 17 Suture 234 3 (100) None 1 (33.3)
2015 Kyuno et al. [14] 2 12.5 Suture 131 0 (0) None 0 (0)
[15]
2016 Ichikawa et al. 12 22 Suture 322 10 (83.3) None 2 (16.7)
2018 Ojima et al. [20] 18 18 (median) Suture 116.5 (median) 4 (38.9) None 0 (0)
Our study 5 23.4 Suture + clips 264 2 (40) Yes 1 (20)
*The final diagnosis of both cases was carcinoid tumors. No. of cancer (%) indicates the number of cases with cancer in the final diagnosis
and its rate of incidence. No. of postoperative complications (%) indicates the number of cases with postoperative complications and its
rate of incidence. Postoperative complications were occasionally documented in previous reports, but treated conservatively (C-D: Grade
II or IIIa). LECS: laparoscopic and endoscopic cooperative surgery; NADENs: non-ampullary duodenal epithelial neoplasms; C-D: Clavien-
Dindo Classification
DISCUSSION
In this study, we present our initial experience of LECS for NADENs, which was accomplished in four out
of the consecutive five cases. We did not experience serious intra- and postoperative complications (> C-D:
Grade IIIb) or tumor recurrence, thereby suggesting the feasibility of our LECS procedure for NADENs,
although the results from our small number of case series study remain limited. In our series of cases suc-
cessfully treated by LECS, early resumption of food intake and full daily activity approximately one week
in the postoperative course demonstrated the reduced invasiveness of our LECS procedure for NADENs.
There was one case of open conversion due to the relatively large mucosal defect (tumor size: 54 mm ×
47 mm in case 5) resulting from ESD in this study, implying the limitation of the indication of our proce-
[17]
dure for LECS for NADENs. Abe et al. reported the successful treatment of duodenal GIST, 62 mm in di-
ameter by laparoscopy-assisted full-thickness resection, where both resection of the lesion and subsequent
repair was performed manually under the 5 to 7 cm upper median laparotomy, suggesting the promising