Page 373 - Read Online
P. 373
Sommariva Liver metastases and HIPEC
Table 2: Studies comparing outcomes of CS + HIPEC alone vs. CS + HIPEC + LR in peritoneal carcinomatosis with
or without liver metastases from colorectal cancer
Follow-up 2-year 3-year 4-year 5-year Median Morbidity Mortality Prognostic
Studies (months) survival survival survival survival survival (%) (%) factors
(%) (%) (%) (%) (months)
Wake Forest 20.7 vs. 13.4 43.3 vs. 26.8 NR 14.4% vs. NR 23.0 vs. 15.8 40.1 vs. 57.1 7.1 vs. 7.7 NR
University 17.4%
Winston-Salem,
USA [29]
Uppsala 45 vs. 57 NR 47 vs. 30 NR NR 34.0 vs. 15 27 vs. 27 9.0 vs. 0 R1 resection
University,
Sweden [30]
Gustave- 62.4 NR 54 vs. 36.5 NR 43.6 vs. 26.4 NR 17 vs. 41 4.2 vs. 8.1 PCI, number
Roussy Institute, of LM, type of
France [20] surgery
St George 19 65 vs. 68 NR NR NR 22.1 38.5 vs. 12.5 0 NR
Hospital, Sidney,
Australia [31]
Université 34.2 89.5 vs. 70.2 NR NR NR 59.2 15.4 vs. 32 0 vs. 4 NR
Catholique
de Louvain,
Belgium [32]
CS: cytoreductive surgery; HIPEC: hyperthermic intraperitoneal chemotherapy; LR: liver resection; PCI: peritoneal cancer index; LM: liver
metastases; NR: not reported
mortality rates less than 2%, comparable to those
observed after surgery for rectal cancer [34,35] . CS +
HIPEC + LR does not seem to give an additional risk
of complication as the morbidity and mortality seems
similar with respect to CS + HIPEC alone [20,29-32] [Table 2].
No study has reported a clear distinction between
complication/mortality rate related to the liver resection
or to the cytoreductive surgery. It should be underlined,
however, that the reported LR combined with CS +
HIPEC are classified as minor procedures, normally
associated with lower risk of complications. Although no
liver specific complications (biloma, bleeding, abscess)
are generally reported, a higher risk of systemic toxicity
has been noted after major LR [36] ; the hypothesis
that transient liver failure leads to a decreased drug
inactivation and therefore a higher systemic toxicity
should be further tested.
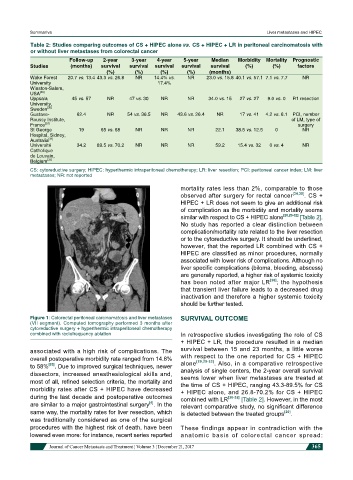
Figure 1: Colorectal peritoneal carcinomatosis and liver metastases SURVIVAL OUTCOME
(VII segment). Computed tomography performed 3 months after
cytoreductive surgery + hyperthermic intraperitoneal chemotherapy
combined with radiofrequency ablation In retrospective studies investigating the role of CS
+ HIPEC + LR, the procedure resulted in a median
associated with a high risk of complications. The survival between 15 and 23 months, a little worse
overall postoperative morbidity rate ranged from 14.8% with respect to the one reported for CS + HIPEC
[20,29-32]
to 58% [33] . Due to improved surgical techniques, newer alone . Also, in a comparative retrospective
dissectors, increased anesthesiological skills and, analysis of single centers, the 2-year overall survival
seems lower when liver metastases are treated at
most of all, refined selection criteria, the mortality and the time of CS + HIPEC, ranging 43.3-89.5% for CS
morbidity rates after CS + HIPEC have decreased + HIPEC alone, and 26.8-70.2% for CS + HIPEC
during the last decade and postoperative outcomes combined with LR [30-32] [Table 2]. However, in the most
[4]
are similar to a major gastrointestinal surgery . In the relevant comparative study, no significant difference
same way, the mortality rates for liver resection, which is detected between the treated groups [20] .
was traditionally considered as one of the surgical
procedures with the highest risk of death, have been These findings appear in contradiction with the
lowered even more: for instance, recent series reported anatomic basis of colorectal cancer spread:
Journal of Cancer Metastasis and Treatment ¦ Volume 3 ¦ December 21, 2017 365