Page 508 - Read Online
P. 508
Yip et al. Hepatoma Res 2020;6:44 I http://dx.doi.org/10.20517/2394-5079.2020.30 Page 3 of 8
Figure 1. Contrast-enhanced computed tomography at 3 months after stereotactic body radiotherapy showing reactive hyperaemia in the
surrounding irradiated non-tumourous liver parenchyma
A
B
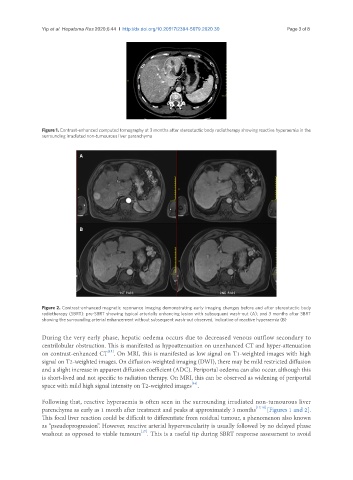
Figure 2. Contrast-enhanced magnetic resonance imaging demonstrating early imaging changes before and after stereotactic body
radiotherapy (SBRT): pre-SBRT showing typical arterially enhancing lesion with subsequent wash-out (A); and 3 months after SBRT
showing the surrounding arterial enhancement without subsequent wash-out observed, indicative of reactive hyperaemia (B)
During the very early phase, hepatic oedema occurs due to decreased venous outflow secondary to
centrilobular obstruction. This is manifested as hypoattenuation on unenhanced CT and hyper-attenuation
[15]
on contrast-enhanced CT . On MRI, this is manifested as low signal on T1-weighted images with high
signal on T2-weighted images. On diffusion-weighted imaging (DWI), there may be mild restricted diffusion
and a slight increase in apparent diffusion coefficient (ADC). Periportal oedema can also occur, although this
is short-lived and not specific to radiation therapy. On MRI, this can be observed as widening of periportal
space with mild high signal intensity on T2-weighted images .
[16]
Following that, reactive hyperaemia is often seen in the surrounding irradiated non-tumourous liver
parenchyma as early as 1 month after treatment and peaks at approximately 3 months [17,18] [Figures 1 and 2].
This focal liver reaction could be difficult to differentiate from residual tumour, a phenomenon also known
as “pseudoprogression”. However, reactive arterial hypervascularity is usually followed by no delayed phase
washout as opposed to viable tumours . This is a useful tip during SBRT response assessment to avoid
[17]