Page 277 - Read Online
P. 277
Kilburn et al. Laparoscopic resection of HCC
laparoscopic compared to open liver resection in the Laparoscopy is also associated with less blood loss
setting of cirrhosis. In the current study, 65% of patients and subsequent need for blood transfusion compared
had cirrhosis (33 Child-Pugh A, 1 Child-Pugh B). There to open surgery, [28,29,31] possibly due to the tamponade
was a trend toward more segmental and subsegmental effect of pneumoperitoneum on the exposed veins
resections in cirrhotics compared to those without and intra-abdominal varices. To reduce blood loss,
cirrhosis. This reflects the desire to spare parenchyma pneumoperitoneum can be transiently increased
to reduce post-operative liver insufficiency, but this to pressures of 16-20 mmHg during parenchymal
needs to be balanced against obtaining adequate transection. Despite concerns over the risk of CO 2
margins, resecting the “oncological territory” of the embolism and respiratory compromise during high-
tumor, and minimizing blood loss and bile leak. Recent pneumoperitoneum, this was not a feature in our series.
publications have suggested that anatomic resection Laparoscopic ultrasound guidance assists in identifying
should be the norm due to the proclivity of HCC to major vascular structures during transection, but the
invade the vasculature and metastasize within the sensitivity of intraoperative ultrasound in localizing
liver. However, the heterogeneity with regards to the small tumors is reduced in cirrhosis.
presence of cirrhosis may be a confounding factor. [22-24]
For parenchymal transection, we favor the use of the
One patient with Child-Pugh B cirrhosis underwent a LigaSure which combines the sealing ability of bipolar
laparoscopic left lateral sectionectomy. This patient coagulation forceps and recapitulates acrush-clamping
died within 30 postoperative days due to postoperative technique. Laparoscopic staplers were used mainly for
liver failure. This case occurred early in the series and pedicle control and avoided for parenchymal transection
as a result, Child-Pugh B status remains a relative due to their tendency to tear the cirrhotic liver.
contraindication to surgical resection in our center.
However, other authors have demonstrated good short Ensuring adequate margins is fundamental to the
and long-term outcomes with reasonable safety in well- overall outcome of the surgery and subsequent patient
selected individuals. [25,26] prognosis. Whilst the benefits of digital palpation
in open surgery may be overstated (especially in
Compared to open resection, laparoscopy may cirrhosis), laparoscopy eliminates this capability. [7,32] We
have a number of benefits in the setting of cirrhosis. found the use of laparoscopic ultrasound essential in
Laparoscopy allows for smaller incisions, which may order to determine a precise transection line in relation
lead to less disruption of the abdominal wall collateral to the tumor margin and locate important vascular
circulation and cause less fluid shifts from exposure of structures. [32,33]
the peritoneal cavity. In those series, 3 patients (9%)
with cirrhosis developed postoperative ascites. Post- Straight resection planes are preferred whenever
operative ascites is common after liver resection, possible. This is relatively easy to achieve for a lateral
even when a relatively small amount of parenchyma sectionectomy or a major hepatectomy, dividing the
is resected. Some studies have demonstrated less liver along well defined scissura. However, in cases
postoperative ascites after laparoscopic liver resection of laparoscopic non-anatomical subsegmentectomies,
compared to laparotomy. [27-30] there is a significant risk of undermining the tumor
leading to a positive margin. This is especially true for
tumors with a wider circumference deep to the liver
Overall survival surface. Starting the dissection 2 cm wider, particularly
No cirrhosis
100 Cirrhosis on the side of the tumor nearest to the surgeon, helps
achieve clearance of the deep margin. Angling the
transection away from the tumor may reduce this risk
and we frequently employ metal clips as ultrasound
visible “markers” which are re-checked through the
Survival (%) 50 transection.
Laparoscopic management of liver tumors has been
reported more commonly for lesions located within
the anterolateral segments of the liver. Some centers
consider posterosuperior lesions (segments 1, 4a, 7, 8),
particularly dome lesions adjacent to the hepatic veins
0
0 50 100 150 200 a contraindication for laparoscopic surgery. This is due
Months to limited visualization, difficult angle of attack, and
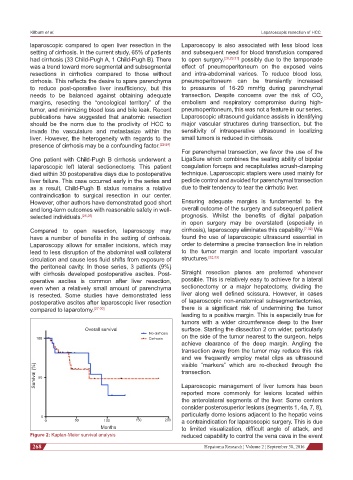
Figure 2: Kaplan-Meier survival analysis reduced capability to control the vena cava in the event
268 Hepatoma Research ¦ Volume 2 ¦ September 30, 2016