Page 29 - Read Online
P. 29
200
150
100
88.8
%
100
50
96
80
0
Survival rate at Survival rate at
7 months 1 year
Group I Group II
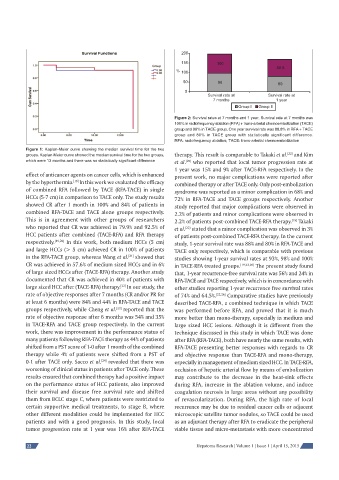
Figure 2: Survival rates at 7 months and 1 year. Survival rate at 7 months was
100% in radiofrequency ablation (RFA) + trans-arterial chemoembolization (TACE)
group and 96% in TACE group. One year survival rate was 88.8% in RFA + TACE
group and 80% in TACE group with statistically significant difference.
RFA: radiofrequency ablation; TACE: trans-arterial chemoembolization
Figure 1: Kaplan-Meier curve showing the median survival time for the two
[22]
groups. Kaplan-Meier curve showed the median survival time for the two groups, therapy. This result is comparable to Takaki et al. and Kim
which were 13 months and there was no statistically signifi cant difference et al. who reported that local tumor progression rate at
[25]
1 year was 15% and 9% after TACE-RFA respectively. In the
effect of anticancer agents on cancer cells, which is enhanced present work, no major complications were reported after
by the hyperthermia. In this work we evaluated the efficacy combined therapy or after TACE only. Only post-embolization
[18]
of combined RFA followed by TACE (RFA-TACE) in single syndrome was reported as a minor complication in 68% and
HCCs (5-7 cm) in comparison to TACE only. The study results 72% in RFA-TACE and TACE groups respectively. Another
showed CR after 1 month in 100% and 84% of patients in study reported that major complications were observed in
combined RFA-TACE and TACE alone groups respectively. 2.2% of patients and minor complications were observed in
This is in agreement with other groups of researchers 2.2% of patients post-combined TACE-RFA therapy. Takaki
[19]
who reported that CR was achieved in 79.9% and 92.5% of et al. stated that a minor complication was observed in 3%
[22]
HCC patients after combined (TACE-RFA) and RFA therapy of patients post-combined TACE-RFA therapy. In the current
respectively. [19,20] In this work, both medium HCCs (5 cm) study, 1-year survival rate was 88% and 80% in RFA-TACE and
and large HCCs (> 5 cm) achieved CR in 100% of patients TACE only respectively, which is comparable with previous
[21]
in the RFA-TACE group, whereas Wang et al. showed that studies showing 1-year survival rates at 93%, 98% and 100%
CR was achieved in 57.6% of medium sized HCCs and in 6% in TACE-RFA treated groups. [19,23,26] The present study found
of large sized HCCs after (TACE-RFA) therapy. Another study that, 1-year recurrence-free survival rate was 56% and 24% in
documented that CR was achieved in 40% of patients with RFA-TACE and TACE respectively, which is in concordance with
large sized HCC after (TACE-RFA) therapy. In our study, the other studies reporting 1-year recurrence free survival rates
[22]
rate of objective responses after 7 months (CR and/or PR for of 74% and 64.5%. [22,26] Comparative studies have previously
at least 6 months) were 84% and 44% in RFA-TACE and TACE described TACE-RFA, a combined technique in which TACE
groups respectively, while Cheng et al. reported that the was performed before RFA, and proved that it is much
[23]
rate of objective response after 6 months was 54% and 35% more better than mono-therapy, especially in medium and
in TACE-RFA and TACE group respectively. In the current large sized HCC lesions. Although it is different from the
work, there was improvement in the performance status of technique discussed in this study in which TACE was done
many patients following RFA-TACE therapy as 44% of patients after RFA (RFA-TACE), both have nearly the same results, with
shifted from a PST score of 1-0 after 1 month of the combined RFA-TACE presenting better responses with regards to CR
therapy while 4% of patients were shifted from a PST of and objective response than TACE-RFA and mono-therapy,
0-1 after TACE only. Sacco et al. revealed that there was especially in management of medium sized HCC. In TACE-RFA,
[24]
worsening of clinical status in patients after TACE only. These occlusion of hepatic arterial flow by means of embolization
results ensured that combined therapy had a positive impact may contribute to the decrease in the heat-sink effects
on the performance status of HCC patients, also improved during RFA, increase in the ablation volume, and induce
their survival and disease free survival rate and shifted coagulation necrosis in large areas without any possibility
them from BCLC stage C, where patients were restricted to of revascularization. During RFA, the high rate of local
certain supportive medical treatments, to stage B, where recurrence may be due to residual cancer cells or adjacent
other different modalities could be implemented for HCC microscopic satellite tumor nodules, so TACE could be used
patients and with a good prognosis. In this study, local as an adjuvant therapy after RFA to eradicate the peripheral
tumor progression rate at 1 year was 16% after RFA-TACE viable tissue and micro-metastasis with more concentrated
22 Hepatoma Research | Volume 1 | Issue 1 | April 15, 2015