Page 35 - Read Online
P. 35
Page 4 of 6 Morise. Hepatoma Res 2020;6:79 I http://dx.doi.org/10.20517/2394-5079.2020.76
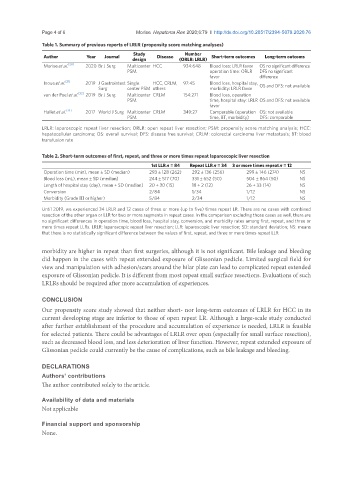
Table 1. Summary of previous reports of LRLR (propensity score matching analyses)
Author Year Journal Study Disease Number Short-term outcomes Long-term outcoms
design (ORLR: LRLR)
Morise et al. [28] 2020 Br J Surg Multicenter HCC 934:648 Blood loss: LRLR favor OS no significant difference
PSM operation time: ORLR DFS no significant
favor difference
Inoue et al. [31] 2019 J Gastrointest Single HCC, CRLM, 97:45 Blood loss, hospital stay, OS and DFS: not available
Surg center PSM others morbidity: LRLR favor
van der Poel et al. [32] 2019 Br J Surg Multicenter CRLM 154:271 Blood loss, operation
PSM time, hospital stay: LRLR OS and DFS: not available
favor
Hallet et al. [33] 2017 World J Surg Multicenter CRLM 349:27 Comparable (operation OS: not available
PSM time, BT, morbidity) DFS: comparable
LRLR: laparoscopic repeat liver resection; ORLR: open repeat liver resection; PSM: propensity score matching analysis; HCC:
hepatocellular carcinoma; OS: overall survival; DFS: disease free survival; CRLM: colorectal carcinoma liver metastasis; BT: blood
transfusion rate
Table 2. Short-term outcomes of first, repeat, and three or more times repeat laparoscopic liver resection
1st LLR n = 84 Repeat LLR n = 34 3 or more times repeat n = 12
Operation time (min), mean ± SD (median) 293 ± 128 (262) 292 ± 136 (256) 299 ± 146 (274) NS
Blood loss (mL), mean ± SD (median) 244 ± 517 (70) 331 ± 652 (50) 504 ± 864 (50) NS
Length of hospital stay (day), mean ± SD (median) 20 ± 30 (15) 18 ± 2 (12) 26 ± 33 (14) NS
Conversion 2/84 1/34 1/12 NS
Morbidity (Grade III or higher) 5/84 2/34 1/12 NS
Until 2019, we experienced 34 LRLR and 12 cases of three or more (up to five) times repeat LR. There are no cases with combined
resection of the other organ or LLR for two or more segments in repeat cases. In the comparison excluding those cases as well, there are
no significant differences in operation time, blood loss, hospital stay, conversion, and morbidity rates among first, repeat, and three or
more times repeat LLRs. LRLR: laparoscopic repeat liver resection; LLR: laparoscopic liver resection; SD: standard deviation; NS: means
that there is no statistically significant difference between the values of first, repeat, and three or more times repeat LLR
morbidity are higher in repeat than first surgeries, although it is not significant. Bile leakage and bleeding
did happen in the cases with repeat extended exposure of Glissonian pedicle. Limited surgical field for
view and manipulation with adhesion/scars around the hilar plate can lead to complicated repeat extended
exposure of Glissonian pedicle. It is different from most repeat small surface resections. Evaluations of such
LRLRs should be required after more accumulation of experiences.
CONCLUSION
Our propensity score study showed that neither short- nor long-term outcomes of LRLR for HCC in its
current developing stage are inferior to those of open repeat LR. Although a large-scale study conducted
after further establishment of the procedure and accumulation of experience is needed, LRLR is feasible
for selected patients. There could be advantages of LRLR over open (especially for small surface resection),
such as decreased blood loss, and less deterioration of liver function. However, repeat extended exposure of
Glissonian pedicle could currently be the cause of complications, such as bile leakage and bleeding.
DECLARATIONS
Authors’ contributions
The author contributed solely to the article.
Availability of data and materials
Not applicable
Financial support and sponsorship
None.