Page 250 - Read Online
P. 250
Seko. Vessel Plus 2020;4:22 I http://dx.doi.org/10.20517/2574-1209.2020.14 Page 3 of 7
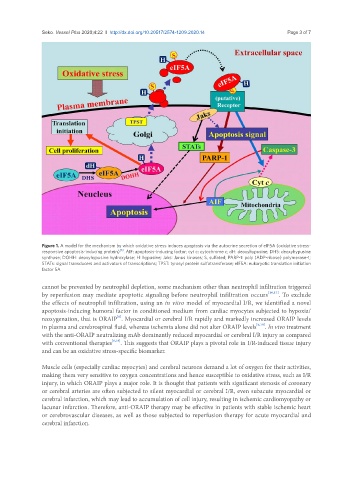
Figure 1. A model for the mechanism by which oxidative stress induces apoptosis via the autocrine secretion of eIF5A (oxidative stress-
[6]
responsive apoptosis-inducing protein) . AIF: apoptosis-inducing factor; cyt c: cytochrome c; dH: deoxyhypusine; DHS: deoxyhypusine
synthase; DOHH: deoxyhypusine hydroxylase; H: hypusine; Jaks: Janus kinases; S, sulfated; PARP-1: poly (ADP-ribose) polymerase-1;
STATs: signal transducers and activators of transcriptions; TPST: tyrosyl protein sulfotransferase; eIF5A: eukaryotic translation initiation
factor 5A
cannot be prevented by neutrophil depletion, some mechanism other than neutrophil infiltration triggered
by reperfusion may mediate apoptotic signaling before neutrophil infiltration occurs [16,17] . To exclude
the effects of neutrophil infiltration, using an in vitro model of myocardial I/R, we identified a novel
apoptosis-inducing humoral factor in conditioned medium from cardiac myocytes subjected to hypoxia/
[6]
reoxygenation, that is ORAIP . Myocardial or cerebral I/R rapidly and markedly increased ORAIP levels
in plasma and cerebrospinal fluid, whereas ischemia alone did not alter ORAIP levels [6,18] . In vivo treatment
with the anti-ORAIP neutralizing mAb dominantly reduced myocardial or cerebral I/R injury as compared
with conventional therapies [6,18] . This suggests that ORAIP plays a pivotal role in I/R-induced tissue injury
and can be an oxidative stress-specific biomarker.
Muscle cells (especially cardiac myocytes) and cerebral neurons demand a lot of oxygen for their activities,
making them very sensitive to oxygen concentrations and hence susceptible to oxidative stress, such as I/R
injury, in which ORAIP plays a major role. It is thought that patients with significant stenosis of coronary
or cerebral arteries are often subjected to silent myocardial or cerebral I/R, even subacute myocardial or
cerebral infarction, which may lead to accumulation of cell injury, resulting in ischemic cardiomyopathy or
lacunar infarction. Therefore, anti-ORAIP therapy may be effective in patients with stable ischemic heart
or cerebrovascular diseases, as well as those subjected to reperfusion therapy for acute myocardial and
cerebral infarction.