Page 81 - Read Online
P. 81
Squizzato et al. Vessel Plus 2023;7:16 https://dx.doi.org/10.20517/2574-1209.2023.05 Page 9 of 14
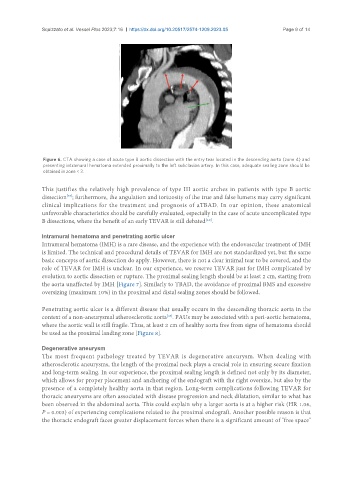
Figure 6. CTA showing a case of acute type B aortic dissection with the entry tear located in the descending aorta (zone 4) and
presenting intramural hematoma extended proximally to the left subclavian artery. In this case, adequate sealing zone should be
obtained in zone < 3.
This justifies the relatively high prevalence of type III aortic arches in patients with type B aortic
dissection ; furthermore, the angulation and tortuosity of the true and false lumens may carry significant
[37]
clinical implications for the treatment and prognosis of aTBAD. In our opinion, these anatomical
unfavorable characteristics should be carefully evaluated, especially in the case of acute uncomplicated type
B dissections, where the benefit of an early TEVAR is still debated .
[1,2]
Intramural hematoma and penetrating aortic ulcer
Intramural hematoma (IMH) is a rare disease, and the experience with the endovascular treatment of IMH
is limited. The technical and procedural details of TEVAR for IMH are not standardized yet, but the same
basic concepts of aortic dissection do apply. However, there is not a clear intimal tear to be covered, and the
role of TEVAR for IMH is unclear. In our experience, we reserve TEVAR just for IMH complicated by
evolution to aortic dissection or rupture. The proximal sealing length should be at least 2 cm, starting from
the aorta unaffected by IMH [Figure 7]. Similarly to TBAD, the avoidance of proximal BMS and excessive
oversizing (maximum 10%) in the proximal and distal sealing zones should be followed.
Penetrating aortic ulcer is a different disease that usually occurs in the descending thoracic aorta in the
context of a non-aneurysmal atherosclerotic aorta . PAUs may be associated with a peri-aortic hematoma,
[38]
where the aortic wall is still fragile. Thus, at least 2 cm of healthy aorta free from signs of hematoma should
be used as the proximal landing zone [Figure 8].
Degenerative aneurysm
The most frequent pathology treated by TEVAR is degenerative aneurysm. When dealing with
atherosclerotic aneurysms, the length of the proximal neck plays a crucial role in ensuring secure fixation
and long-term sealing. In our experience, the proximal sealing length is defined not only by its diameter,
which allows for proper placement and anchoring of the endograft with the right oversize, but also by the
presence of a completely healthy aorta in that region. Long-term complications following TEVAR for
thoracic aneurysms are often associated with disease progression and neck dilatation, similar to what has
been observed in the abdominal aorta. This could explain why a larger aorta is at a higher risk (HR 1.06,
P = 0.003) of experiencing complications related to the proximal endograft. Another possible reason is that
the thoracic endograft faces greater displacement forces when there is a significant amount of "free space"