Page 53 - Read Online
P. 53
Othman et al. Plast Aesthet Res 2022;9:29 https://dx.doi.org/10.20517/2347-9264.2021.135 Page 7 of 10
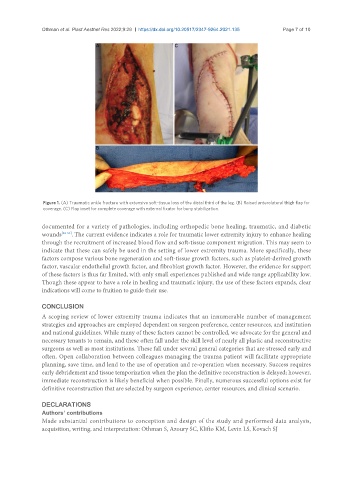
Figure 1. (A) Traumatic ankle fracture with extensive soft-tissue loss of the distal third of the leg. (B) Raised anterolateral thigh flap for
coverage. (C) Flap inset for complete coverage with external fixator for bony stabilization.
documented for a variety of pathologies, including orthopedic bone healing, traumatic, and diabetic
wounds [53-55] . The current evidence indicates a role for traumatic lower extremity injury to enhance healing
through the recruitment of increased blood flow and soft-tissue component migration. This may seem to
indicate that these can safely be used in the setting of lower extremity trauma. More specifically, these
factors compose various bone regeneration and soft-tissue growth factors, such as platelet-derived growth
factor, vascular endothelial growth factor, and fibroblast growth factor. However, the evidence for support
of these factors is thus far limited, with only small experiences published and wide range applicability low.
Though these appear to have a role in healing and traumatic injury, the use of these factors expands, clear
indications will come to fruition to guide their use.
CONCLUSION
A scoping review of lower extremity trauma indicates that an innumerable number of management
strategies and approaches are employed dependent on surgeon preference, center resources, and institution
and national guidelines. While many of these factors cannot be controlled, we advocate for the general and
necessary tenants to remain, and these often fall under the skill level of nearly all plastic and reconstructive
surgeons as well as most institutions. These fall under several general categories that are stressed early and
often. Open collaboration between colleagues managing the trauma patient will facilitate appropriate
planning, save time, and lend to the use of operation and re-operation when necessary. Success requires
early debridement and tissue temporization when the plan the definitive reconstruction is delayed; however,
immediate reconstruction is likely beneficial when possible. Finally, numerous successful options exist for
definitive reconstruction that are selected by surgeon experience, center resources, and clinical scenario.
DECLARATIONS
Authors’ contributions
Made substantial contributions to conception and design of the study and performed data analysis,
acquisition, writing, and interpretation: Othman S, Azoury SC, Klifto KM, Levin LS, Kovach SJ