Page 118 - Read Online
P. 118
Mayland et al. Plast Aesthet Res 2021;8:62 https://dx.doi.org/10.20517/2347-9264.2021.38 Page 7 of 10
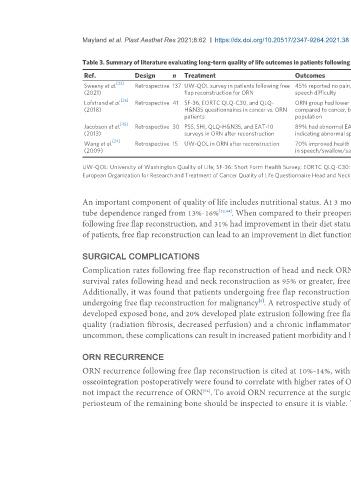
Table 3. Summary of literature evaluating long-term quality of life outcomes in patients following microvascular reconstruction of osteonecrosis defects
Ref. Design n Treatment Outcomes Conclusion
[22]
Sweeny et al. Retrospective 137 UW-QOL survey in patients following free 45% reported no pain, 28% no swallowing abnormalities, 93% no Data suggests a good return of function and QOL
(2021) flap reconstruction for ORN speech difficulty following surgery
[26]
Lofstrand et al. Retrospective 41 SF-36, EORTC QLQ-C30, and QLQ- ORN group had lower scores in swallowing and social eating Cancer and ORN patients have similar QOL following
(2018) H&N35 questionnaires in cancer vs. ORN compared to cancer, but general QOL did not differ from the reference reconstruction with the exception of swallowing/social
patients population eating
[45]
Jacobson et al. Retrospective 30 PSS, SHI, QLQ-H&N35, and EAT-10 89% had abnormal EAT-10 and SHI scores following reconstruction, Many patients remain unhappy with speech and
(2013) surveys in ORN after reconstruction indicating abnormal speech and swallow swallowing outcomes following reconstruction
[24]
Wang et al. Retrospective 15 UW-QOL in ORN after reconstruction 70% improved health related QOL after reconstruction, lowest scores Best scores in pain, but patients still have QOL issues
(2009) in speech/swallow/saliva with speech, swallow, and saliva
UW-QOL: University of Washington Quality of Life; SF-36: Short Form Health Survey; EORTC QLQ-C30: European Organization for Research and Treatment of Cancer quality of life questionnaire; QLQ-H&N35:
European Organization for Research and Treatment of Cancer Quality of Life Questionnaire Head and Neck Module; PSS: Performance Status Scale; SHI: Speech Handicap Index; EAT-10: Eating Assessment Tool.
An important component of quality of life includes nutritional status. At 3 months following free flap reconstruction for advanced ORN, the rates of feeding
tube dependence ranged from 13%-16% [22,44] . When compared to their preoperative nutritional status, 47% of patients were tolerating a regular diet at 5 years
following free flap reconstruction, and 31% had improvement in their diet status following free flap reconstructive surgery . This data suggest that for a subset
[22]
of patients, free flap reconstruction can lead to an improvement in diet function.
SURGICAL COMPLICATIONS
Complication rates following free flap reconstruction of head and neck ORN are cited between 30%-60% [16,26,44,46,49,50] . While most institutions cite free flap
survival rates following head and neck reconstruction as 95% or greater, free flap survival rates following ORN reconstruction are cited at 89-93% [26,46,50,51] .
Additionally, it was found that patients undergoing free flap reconstruction for ORN had a higher incidence of late complications compared to patients
undergoing free flap reconstruction for malignancy . A retrospective study of 277 patients found that 24% of patients developed a postoperative fistula, 16%
[3]
developed exposed bone, and 20% developed plate extrusion following free flap reconstruction for ORN . These complications are attributed to poor tissue
[40]
quality (radiation fibrosis, decreased perfusion) and a chronic inflammatory reaction in response to persistent infection and saliva exposure. Although
uncommon, these complications can result in increased patient morbidity and healthcare costs [50,52,53] .
ORN RECURRENCE
ORN recurrence following free flap reconstruction is cited at 10%-14%, with a median time to onset of 11 months [17,22] . Poor wound healing and failure of
[22]
osseointegration postoperatively were found to correlate with higher rates of ORN recurrence . While the donor site selected for free flap reconstruction did
not impact the recurrence of ORN . To avoid ORN recurrence at the surgical site, every attempt should be made to resect necrotic non-viable bone. The
[54]
periosteum of the remaining bone should be inspected to ensure it is viable. The periosteum is a dense fibrous membrane with a rich vascular supply that