Page 629 - Read Online
P. 629
Page 2 of 6 Dharmaraj et al. Mini-invasive Surg 2020;4:65 I http://dx.doi.org/10.20517/2574-1225.2020.51
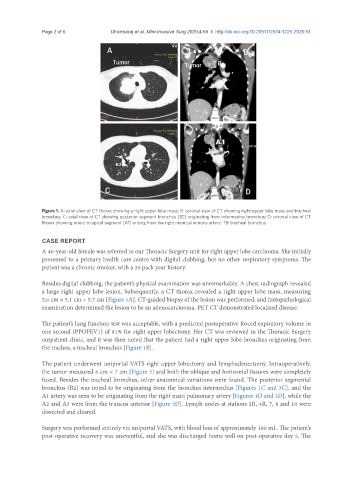
Figure 1. A: axial view of CT thorax showing a right upper lobe mass; B: coronal view of CT showing right upper lobe mass and tracheal
bronchus; C: axial view of CT showing posterior segment bronchus (B2) originating from intermedius bronchus; D: coronal view of CT
thorax showing artery to apical segment (A1) arising from the right main pulmonary artery. TB: tracheal bronchus
CASE REPORT
A 40-year-old female was referred to our Thoracic Surgery unit for right upper lobe carcinoma. She initially
presented to a primary health care centre with digital clubbing, but no other respiratory symptoms. The
patient was a chronic smoker, with a 20 pack year history.
Besides digital clubbing, the patient’s physical examination was unremarkable. A chest radiograph revealed
a large right upper lobe lesion. Subsequently, a CT thorax revealed a right upper lobe mass, measuring
5.6 cm × 5.1 cm × 5.7 cm [Figure 1A]. CT-guided biopsy of the lesion was performed, and histopathological
examination determined the lesion to be an adenocarcinoma. PET CT demonstrated localized disease.
The patient’s lung function test was acceptable, with a predicted postoperative forced expiratory volume in
one second (PPOFEV1) of 81% for right upper lobectomy. Her CT was reviewed in the Thoracic Surgery
outpatient clinic, and it was then noted that the patient had a right upper lobe bronchus originating from
the trachea, a tracheal bronchus [Figure 1B].
The patient underwent uniportal VATS right upper lobectomy and lymphadenectomy. Intraoperatively,
the tumor measured 6 cm × 7 cm [Figure 2] and both the oblique and horizontal fissures were completely
fused. Besides the tracheal bronchus, other anatomical variations were found. The posterior segmental
bronchus (B2) was noted to be originating from the bronchus intermedius [Figures 1C and 3C], and the
A1 artery was seen to be originating from the right main pulmonary artery [Figures 1D and 3D], while the
A2 and A3 were from the truncus anterior [Figure 3D]. Lymph nodes at stations 2R, 4R, 7, 8 and 10 were
dissected and cleared.
Surgery was performed entirely via uniportal VATS, with blood loss of approximately 100 mL. The patient’s
post-operative recovery was uneventful, and she was discharged home well on post-operative day 5. The