Page 133 - Read Online
P. 133
Page 4 of 8 Shibao et al. Mini-invasive Surg 2019;3:16 I http://dx.doi.org/10.20517/2574-1225.2019.01
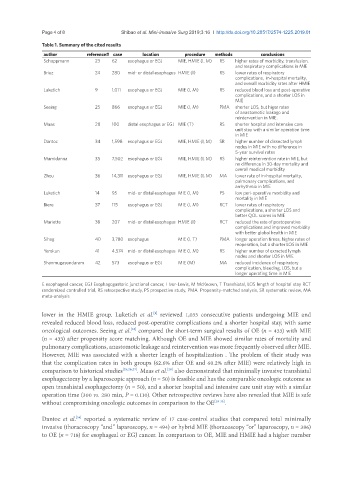
Table 1. Summary of the cited results
author reference# case location procedure methods conclusions
Schoppmann 23 62 esophagus or EGJ MIE, HMIE (I, M) RS higher rates of morbidity, transfusion,
and respiratory complications in MIE
Briez 24 280 mid- or distal esophagus HMIE (I) RS lower rates of respiratory
complications, in-hospital mortality,
and overall morbidity rates after HMIE
Luketich 9 1,011 esophagus or EGJ MIE (I, M) RS reduced blood loss and post-operative
complications, and a shorter LOS in
MIE
Seeing 25 866 esophagus or EGJ MIE (I, M) PMA shorter LOS, but higer rates
of anastomotic leakage and
reintervention in MIE.
Maas 28 100 distal esophagus or EGJ MIE (T) RS shorter hospital and intensive care
unit stay with a similar operation time
in MIE
Dantoc 34 1,598 esophagus or EGJ MIE, HMIE (I, M) SR higher number of dissected lymph
nodes in MIE with no difference in
5-year survival rates
Mamidanna 35 7,502 esophagus or EGJ MIE, HMIE (I, M) RS higher reintervention rate in MIE, but
no difference in 30-day mortality and
overall medical morbidity
Zhou 36 14,311 esophagus or EGJ MIE, HMIE (I, M) MA lower rate of in-hospital mortality,
pulmonary complications, and
arrhythmia in MIE
Luketich 14 95 mid- or distal esophagus MIE (I, M) PS low peri-operative morbidity and
mortality in MIE
Biere 37 115 esophagus or EGJ MIE (I, M) RCT lower rates of respiratory
complications, a shorter LOS and
better QOL scores in MIE
Mariette 38 207 mid- or distal esophagus HMIE (I) RCT reduced the rate of postoperative
complications and improved morbidity
with better global health in MIE
Sihag 40 3,780 esophagus MIE (I, T) PMA longer operation times, higher rates of
reoperation, but a shorter LOS in MIE
Yerokun 41 4,574 mid- or distal esophagus MIE (I, M) RS higher number of exracted lymph
nodes and shorter LOS in MIE
Shanmugasundaram 42 573 esophagus or EGJ MIE (M) MA reduced incidence of respiratory
complication, bleeding, LOS, but a
longer operating time in MIE
E esophageal cancer, EGJ Esophagogastoric junctional cancer, I Ivor-Lewis, M McKeown, T Transhiatal, LOS length of hospital stay RCT
randomized controlled trial, RS retrospective study, PS prospective study, PMA Propensity-matched analysis, SR systematic review, MA
meta-analysis
lower in the HMIE group. Luketich et al. reviewed 1,033 consecutive patients undergoing MIE and
[9]
revealed reduced blood loss, reduced post-operative complications and a shorter hospital stay, with same
oncological outcomes. Seeing et al. compared the short-term surgical results of OE (n = 433) with MIE
[25]
(n = 433) after propensity score matching. Although OE and MIE showed similar rates of mortality and
pulmonary complications, anastomotic leakage and reintervention was more frequently observed after MIE.
However, MIE was associated with a shorter length of hospitalization . The problem of their study was
that the complication rates in both groups (62.6% after OE and 60.2% after MIE) were relatively high in
comparison to historical studies [25,26,27] . Maas et al. also demonstrated that minimally invasive transhiatal
[28]
esophagectomy by a laparoscopic approach (n = 50) is feasible and has the comparable oncologic outcome as
open transhiatal esophagectomy (n = 50), and a shorter hospital and intensive care unit stay with a similar
operation time (300 vs. 280 min, P = 0.110). Other retrospective reviews have also revealed that MIE is safe
without compromising oncologic outcomes in comparison to the OE [29-33] .
Dantoc et al. reported a systematic review of 17 case-control studies that compared total minimally
[34]
invasive (thoracoscopy “and” laparoscopy, n = 494) or hybrid MIE (thoracoscopy “or” laparoscopy, n = 386)
to OE (n = 718) for esophageal or EGJ cancer. In comparison to OE, MIE and HMIE had a higher number