Page 372 - Read Online
P. 372
Marasco et al. Hepatoma Res 2020;6:33 I http://dx.doi.org/10.20517/2394-5079.2020.01 Page 7 of 19
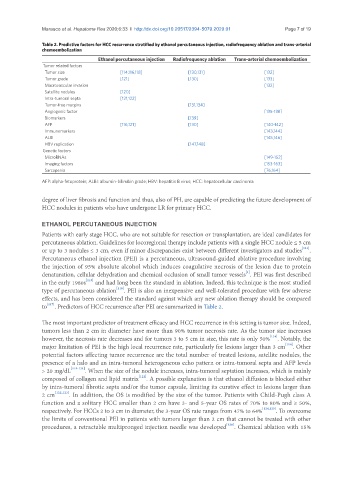
Table 2. Predictive factors for HCC recurrence stratified by ethanol percutaneous injection, radiofrequency ablation and trans-arterial
chemoembolization
Ethanol percutaneous injection Radiofrequency ablation Trans-arterial chemoembolization
Tumor related factors
Tumor size [114,116,118] [130,131] [132]
Tumor grade [121] [130] [133]
Macrovascular invasion [132]
Satellite nodules [120]
Intra-tumoral septa [121,122]
Tumor-free margins [131,134]
Angiogenic factor [135-138]
Biomarkers [139]
AFP [116,121] [130] [140-142]
Immunomarkers [143,144]
ALBI [145,146]
HBV replication [147,148]
Genetic factors
MicroRNAs [149-152]
Imaging factors [153-163]
Sarcopenia [76,164]
AFP: alpha-fetoprotein; ALBI: albumin-bilirubin grade; HBV: hepatitis B virus; HCC: hepatocellular carcinoma
degree of liver fibrosis and function and thus, also of PH, are capable of predicting the future development of
HCC nodules in patients who have undergone LR for primary HCC.
ETHANOL PERCUTANEOUS INJECTION
Patients with early stage HCC, who are not suitable for resection or transplantation, are ideal candidates for
percutaneous ablation. Guidelines for locoregional therapy include patients with a single HCC nodule ≤ 5 cm
or up to 3 nodules ≤ 3 cm, even if minor discrepancies exist between different investigators and studies [114] .
Percutaneous ethanol injection (PEI) is a percutaneous, ultrasound-guided ablative procedure involving
the injection of 95% absolute alcohol which induces coagulative necrosis of the lesion due to protein
[1]
denaturation, cellular dehydration and chemical occlusion of small tumor vessels . PEI was first described
in the early 1980s [115] and had long been the standard in ablation. Indeed, this technique is the most studied
type of percutaneous ablation [116] . PEI is also an inexpensive and well-tolerated procedure with few adverse
effects, and has been considered the standard against which any new ablation therapy should be compared
to [117] . Predictors of HCC recurrence after PEI are summarized in Table 2.
The most important predictor of treatment efficacy and HCC recurrence in this setting is tumor size. Indeed,
tumors less than 2 cm in diameter have more than 90% tumor necrosis rate. As the tumor size increases
however, the necrosis rate decreases and for tumors 3 to 5 cm in size, this rate is only 50% [114] . Notably, the
major limitation of PEI is the high local recurrence rate, particularly for lesions larger than 3 cm [118] . Other
potential factors affecting tumor recurrence are the total number of treated lesions, satellite nodules, the
presence of a halo and an intra-tumoral heterogeneous echo pattern or intra-tumoral septa and AFP levels
> 20 mg/dL [119-121] . When the size of the nodule increases, intra-tumoral septation increases, which is mainly
composed of collagen and lipid matrix [122] . A possible explanation is that ethanol diffusion is blocked either
by intra-tumoral fibrotic septa and/or the tumor capsule, limiting its curative effect in lesions larger than
2 cm [122,123] . In addition, the OS is modified by the size of the tumor. Patients with Child-Pugh class A
function and a solitary HCC smaller than 2 cm have 3- and 5-year OS rates of 70% to 80% and ≥ 50%,
respectively. For HCCs 2 to 3 cm in diameter, the 3-year OS rate ranges from 47% to 64% [124,125] . To overcome
the limits of conventional PEI in patients with tumors larger than 2 cm that cannot be treated with other
procedures, a retractable multipronged injection needle was developed [126] . Chemical ablation with 15%