Page 208 - Read Online
P. 208
Page 8 of 15 Rodrigues et al. Vessel Plus 2024;8:10 https://dx.doi.org/10.20517/2574-1209.2023.109
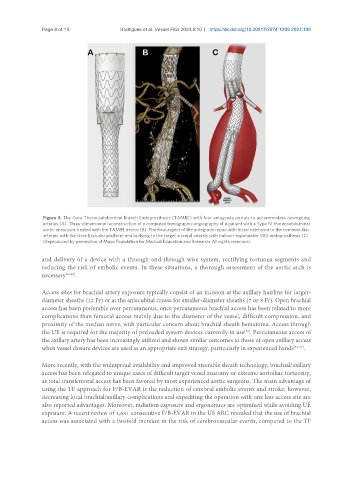
Figure 4. The Gore Thoracoabdominal Branch Endoprosthesis (TAMBE) with four antegrade portals to accommodate downgoing
arteries (A). Three-dimensional reconstruction of a computed tomographic angiography of a patient with a Type IV thoracoabdominal
aortic aneurysm treated with the TAMBE device (B). The final aspect of the antegrade repair with distal extension to the common iliac
arteries with the Gore Excluder platform and bridging to the target visceral vessels with balloon-expandable VBX endoprosthesis (C).
(Reproduced by permission of Mayo Foundation for Medical Education and Research. All rights reserved).
and delivery of a device with a through-and-through wire system, rectifying tortuous segments and
reducing the risk of embolic events. In these situations, a thorough assessment of the aortic arch is
necessary [39,49] .
Access sites for brachial artery exposure typically consist of an incision at the axillary hairline for larger-
diameter sheaths (12 Fr) or at the antecubital crease for smaller-diameter sheaths (7 or 8 Fr). Open brachial
access has been preferable over percutaneous, once percutaneous brachial access has been related to more
complications than femoral access mainly due to the diameter of the vessel, difficult compression, and
proximity of the median nerve, with particular concern about brachial sheath hematoma. Access through
the UE is required for the majority of preloaded system devices currently in use . Percutaneous access of
[50]
the axillary artery has been increasingly utilized and shown similar outcomes to those of open axillary access
when vessel closure devices are used as an appropriate exit strategy, particularly in experienced hands [51-53] .
More recently, with the widespread availability and improved steerable sheath technology, brachial/axillary
access has been relegated to unique cases of difficult target vessel anatomy or extreme aortoiliac tortuosity,
as total transfemoral access has been favored by most experienced aortic surgeons. The main advantage of
using the TF approach for F/B-EVAR is the reduction of cerebral embolic events and stroke; however,
decreasing local brachial/axillary complications and expediting the operation with one less access site are
also reported advantages. Moreover, radiation exposure and ergonomics are optimized while avoiding UE
exposure. A recent review of 1,681 consecutive F/B-EVAR in the US ARC revealed that the use of brachial
access was associated with a twofold increase in the risk of cerebrovascular events, compared to the TF