Page 85 - Read Online
P. 85
Page 10 of 18 Billings et al. Plast Aesthet Res. 2025;12:27 https://dx.doi.org/10.20517/2347-9264.2025.52
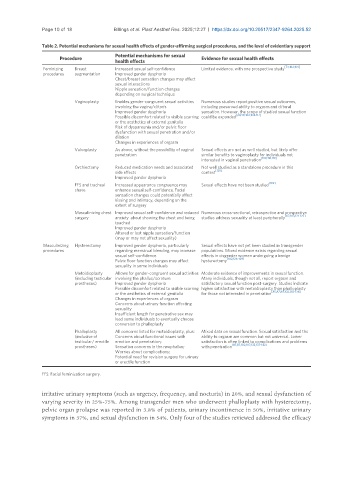
Table 2. Potential mechanisms for sexual health effects of gender-affirming surgical procedures, and the level of evidentiary support
Potential mechanisms for sexual
Procedure Evidence for sexual health effects
health effects
[73,102,103]
Feminizing Breast Increased sexual self-confidence Limited evidence, with one prospective study
procedures augmentation Improved gender dysphoria
Chest/breast sensation changes may affect
sexual interactions
Nipple sensation/function changes
depending on surgical technique
Vaginoplasty Enables gender-congruent sexual activities Numerous studies report positive sexual outcomes,
involving the vagina/clitoris including preserved ability to orgasm and clitoral
Improved gender dysphoria sensation. However, the scope of studied sexual function
[24,30,102,104-117]
Possible discomfort related to visible scarring could be expanded
or the aesthetics of external genitalia
Risk of dyspareunia and/or pelvic floor
dysfunction with sexual penetration and/or
dilation
Changes in experiences of orgasm
Vulvoplasty As above, without the possibility of vaginal Sexual effects are not as well studied, but likely offer
penetration similar benefits to vaginoplasty for individuals not
[108,118,119]
interested in vaginal penetration
Orchiectomy Reduced medication needs and associated Not well studied as a standalone procedure in this
side effects context [120]
Improved gender dysphoria
FFS and tracheal Increased appearance congruence may Sexual effects have not been studied [102]
shave enhance sexual self-confidence. Facial
sensation changes could potentially affect
kissing and intimacy, depending on the
extent of surgery
Masculinizing chest Improved sexual self-confidence and reduced Numerous cross-sectional, retrospective and prospective
[67,103,121-125]
surgery anxiety about showing the chest and being studies address sexuality at least peripherally
touched
Improved gender dysphoria
Altered or lost nipple sensation/function
(may or may not affect sexuality)
Masculinizing Hysterectomy Improved gender dysphoria, particularly Sexual effects have not yet been studied in transgender
procedures regarding menstrual bleeding, may increase populations. Mixed evidence exists regarding sexual
sexual self-confidence effects in cisgender women undergoing a benign
[102,126-129]
Pelvic floor function changes may affect hysterectomy
sexuality in some individuals
Metoidioplasty Allows for gender-congruent sexual activities Moderate evidence of improvements in sexual function.
(including testicular involving the phallus/scrotum Many individuals, though not all, report orgasm and
prostheses) Improved gender dysphoria satisfactory sexual function post-surgery. Studies indicate
Possible discomfort related to visible scarring higher satisfaction with metoidioplasty than phalloplasty
[85,87,89,102,130-136]
or the aesthetics of external genitalia for those not interested in penetration
Changes in experiences of orgasm
Concerns about urinary function affecting
sexuality
Insufficient length for penetrative sex may
lead some individuals to eventually choose
conversion to phalloplasty
Phalloplasty All concerns listed for metoidioplasty, plus: Mixed data on sexual function. Sexual satisfaction and the
(inclusive of Concerns about functional issues with ability to orgasm are common but not universal. Lower
testicular/ erectile erection and penetration; satisfaction is often linked to complications and problems
[87,87,102,107,133,137-142]
prostheses) Sensation concerns in the neophallus; with penetration
Worries about complications;
Potential need for revision surgery for urinary
or erectile function
FFS: Facial feminization surgery.
irritative urinary symptoms (such as urgency, frequency, and nocturia) in 20%, and sexual dysfunction of
varying severity in 25%-75%. Among transgender men who underwent phalloplasty with hysterectomy,
pelvic organ prolapse was reported in 3.8% of patients, urinary incontinence in 50%, irritative urinary
symptoms in 37%, and sexual dysfunction in 54%. Only four of the studies reviewed addressed the efficacy