Page 36 - Read Online
P. 36
Laustsen-Kiel et al. Plast Aesthet Res 2024;11:17 https://dx.doi.org/10.20517/2347-9264.2024.32 Page 7 of 18
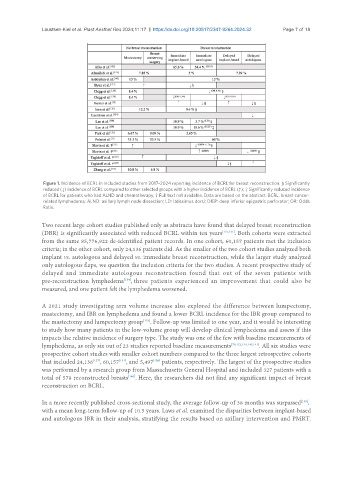
Figure 1. Incidence of BCRL in included studies from 2017-2024 reporting incidence of BCRL for breast reconstruction. § Significantly
reduced (↓) incidence of BCRL compared to other selected groups with a higher incidence of BCRL (↑); ‡ Significantly reduced incidence
of BCRL for patients who had ALND and chemotherapy; † Full text not available. Data are based on the abstract. BCRL: breast cancer-
related lymphedema; ALND: axillary lymph node dissection; LD: latissimus dorsi; DIEP: deep inferior epigastric perforator; OR: Odds
Ratio.
Two recent large cohort studies published only as abstracts have found that delayed breast reconstruction
(DBR) is significantly associated with reduced BCRL within ten years [127,131] . Both cohorts were extracted
from the same 85,776,922 de-identified patient records. In one cohort, 60,157 patients met the inclusion
criteria; in the other cohort, only 24,136 patients did. As the smaller of the two cohort studies analyzed both
implant vs. autologous and delayed vs. immediate breast reconstruction, while the larger study analyzed
only autologous flaps, we question the inclusion criteria for the two studies. A recent prospective study of
delayed and immediate autologous reconstruction found that out of the seven patients with
pre-reconstruction lymphedema , three patients experienced an improvement that could also be
[134]
measured, and one patient felt the lymphedema worsened.
A 2021 study investigating arm volume increase also explored the difference between lumpectomy,
mastectomy, and IBR on lymphedema and found a lower BCRL incidence for the IBR group compared to
the mastectomy and lumpectomy group . Follow-up was limited to one year, and it would be interesting
[129]
to study how many patients in the low-volume group will develop clinical lymphedema and assess if this
impacts the relative incidence of surgery type. The study was one of the few with baseline measurements of
lymphedema, as only six out of 23 studies reported baseline measurements [70,122,134,140,141] . All six studies were
prospective cohort studies with smaller cohort numbers compared to the three largest retrospective cohorts
that included 24,136 , 60,157 , and 5,497 patients, respectively. The largest of the prospective studies
[127]
[131]
[126]
was performed by a research group from Massachusetts General Hospital and included 327 patients with a
total of 578 reconstructed breasts . Here, the researchers did not find any significant impact of breast
[140]
reconstruction on BCRL.
[135]
In a more recently published cross-sectional study, the average follow-up of 38 months was surpassed ,
with a mean long-term follow-up of 10.5 years. Laws et al. examined the disparities between implant-based
and autologous IBR in their analysis, stratifying the results based on axillary intervention and PMRT.