Page 84 - Read Online
P. 84
Page 78 Xu et al. J Transl Genet Genom 2023;7:87-93 https://dx.doi.org/10.20517/jtgg.2023.10
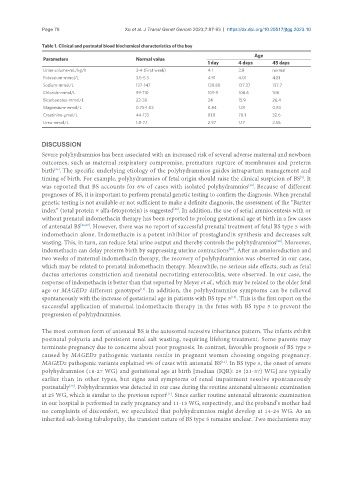
Table 1. Clinical and postnatal blood biochemical characteristics of the boy
Age
Parameters Normal value
1 day 4 days 45 days
Urine volume-mL/kg/h 3-4 (First week) 4.1 3.8 normal
Potassium-mmol/L 3.5-5.3 4.91 4.01 4.81
Sodium-mmol/L 137-147 138.80 137.37 137.7
Chloride-mmol/L 99-110 109.9 108.6 106
Bicarbonates-mmol/L 22-30 24 15.9 26.4
Magnesium-mmol/L 0.75-1.02 0.84 1.01 0.83
Creatinine-μmol/L 44-133 81.8 78.1 32.6
Urea-mmol/L 1.8-7.1 2.97 1.17 2.56
DISCUSSION
Severe polyhydramnios has been associated with an increased risk of several adverse maternal and newborn
outcomes, such as maternal respiratory compromise, premature rupture of membranes and preterm
birth . The specific underlying etiology of the polyhydramnios guides intrapartum management and
[24]
[8]
timing of birth. For example, polyhydramnios of fetal origin should raise the clinical suspicion of BS . It
was reported that BS accounts for 6% of cases with isolated polyhydramnios . Because of different
[25]
prognoses of BS, it is important to perform prenatal genetic testing to confirm the diagnosis. When prenatal
genetic testing is not available or not sufficient to make a definite diagnosis, the assessment of the “Bartter
index” (total protein × alfa-fetoprotein) is suggested . In addition, the use of serial amniocentesis with or
[25]
without prenatal indomethacin therapy has been reported to prolong gestational age at birth in a few cases
of antenatal BS [26,27] . However, there was no report of successful prenatal treatment of fetal BS type 5 with
indomethacin alone. Indomethacin is a potent inhibitor of prostaglandin synthesis and decreases salt
wasting. This, in turn, can reduce fetal urine output and thereby controls the polyhydramnios . Moreover,
[28]
indomethacin can delay preterm birth by suppressing uterine contractions . After an amnioreduction and
[29]
two weeks of maternal indomethacin therapy, the recovery of polyhydramnios was observed in our case,
which may be related to prenatal indomethacin therapy. Meanwhile, no serious side effects, such as fetal
ductus arteriosus constriction and neonatal necrotizing enterocolitis, were observed. In our case, the
response of indomethacin is better than that reported by Meyer et al., which may be related to the older fetal
age or MAGED2 different genotypes . In addition, the polyhydramnios symptoms can be relieved
[13]
spontaneously with the increase of gestational age in patients with BS type 5 . This is the first report on the
[18]
successful application of maternal indomethacin therapy in the fetus with BS type 5 to prevent the
progression of polyhydramnios.
The most common form of antenatal BS is the autosomal recessive inheritance pattern. The infants exhibit
postnatal polyuria and persistent renal salt wasting, requiring lifelong treatment. Some parents may
terminate pregnancy due to concerns about poor prognosis. In contrast, favorable prognosis of BS type 5
caused by MAGED2 pathogenic variants results in pregnant women choosing ongoing pregnancy.
[11]
MAGED2 pathogenic variants explained 9% of cases with antenatal BS . In BS type 5, the onset of severe
polyhydramnios (18-27 WG) and gestational age at birth [median (IQR): 29 (21-37) WG] are typically
earlier than in other types, but signs and symptoms of renal impairment resolve spontaneously
postnatally . Polyhydramnios was detected in our case during the routine antenatal ultrasonic examination
[30]
at 25 WG, which is similar to the previous report . Since earlier routine antenatal ultrasonic examination
[11]
in our hospital is performed in early pregnancy and 11-13 WG, respectively, and the proband’s mother had
no complaints of discomfort, we speculated that polyhydramnios might develop at 14-24 WG. As an
inherited salt-losing tubulopathy, the transient nature of BS type 5 remains unclear. Two mechanisms may