Page 560 - Read Online
P. 560
Page 4 of 8 Puckett et al. J Cancer Metastasis Treat 2020;6:11 I http://dx.doi.org/10.20517/2394-4722.2020.98
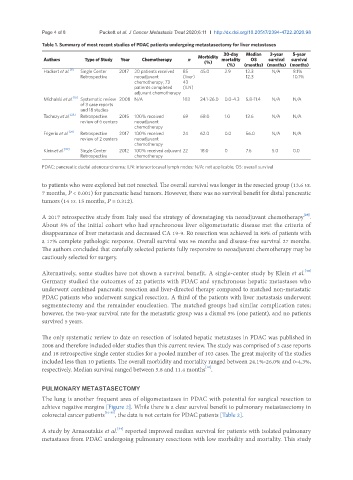
Table 1. Summary of most recent studies of PDAC patients undergoing metastasectomy for liver metastases
30-day Median 2-year 5-year
Morbidity
Authors Type of Study Year Chemotherapy n mortality OS survival survival
(%)
(%) (months) (months) (months)
Hackert et al. Single Center 2017 20 patients received 85 45.0 2.9 12.3 N/A 8.1%
[9]
Retrospective neoadjuvant (liver) 12.3 10.1%
chemotherapy; 73 43
patients completed (ILN)
adjuvant chemotherapy
Michalski et al. [10] Systematic review 2008 N/A 103 24.1-26.0 0.0-4.3 5.8-11.4 N/A N/A
of 3 case reports
and 18 studies
Tachezy et al. [28] Retrospective 2015 100% received 69 68.0 1.0 13.6 N/A N/A
review of 6 centers neoadjuvant
chemotherapy
Frigerio et al. [29] Retrospective 2017 100% received 24 62.0 0.0 56.0 N/A N/A
review of 2 centers neoadjuvant
chemotherapy
Klein et al. [30] Single Center 2012 100% received adjuvant 22 18.0 0 7.6 5.0 0.0
Retrospective chemotherapy
PDAC: pancreatic ductal adenocarcinoma; ILN: interaortocaval lymph nodes; N/A: not applicable; OS: overall survival
to patients who were explored but not resected. The overall survival was longer in the resected group (13.6 vs.
7 months, P < 0.001) for pancreatic head tumors. However, there was no survival benefit for distal pancreatic
tumors (14 vs. 15 months, P = 0.312).
[29]
A 2017 retrospective study from Italy used the strategy of downstaging via neoadjuvant chemotherapy .
About 5% of the initial cohort who had synchronous liver oligometastatic disease met the criteria of
disappearance of liver metastasis and decreased CA 19-9. R0 resection was achieved in 88% of patients with
a 17% complete pathologic response. Overall survival was 56 months and disease-free survival 27 months.
The authors concluded that carefully selected patients fully responsive to neoadjuvant chemotherapy may be
cautiously selected for surgery.
Alternatively, some studies have not shown a survival benefit. A single-center study by Klein et al.
[30]
Germany studied the outcomes of 22 patients with PDAC and synchronous hepatic metastases who
underwent combined pancreatic resection and liver-directed therapy compared to matched non-metastatic
PDAC patients who underwent surgical resection. A third of the patients with liver metastasis underwent
segmentectomy and the remainder enucleation. The matched groups had similar complication rates;
however, the two-year survival rate for the metastatic group was a dismal 5% (one patient), and no patients
survived 5 years.
The only systematic review to date on resection of isolated hepatic metastases in PDAC was published in
2008 and therefore included older studies than this current review. The study was comprised of 3 case reports
and 18 retrospective single center studies for a pooled number of 103 cases. The great majority of the studies
included less than 10 patients. The overall morbidity and mortality ranged between 24.1%-26.0% and 0-4.3%,
[10]
respectively. Median survival ranged between 5.8 and 11.4 months .
PULMONARY METASTASECTOMY
The lung is another frequent area of oligometastases in PDAC with potential for surgical resection to
achieve negative margins [Figure 2]. While there is a clear survival benefit to pulmonary metastasectomy in
colorectal cancer patients [31-35] , the data is not certain for PDAC patients [Table 2].
[34]
A study by Arnaoutakis et al. reported improved median survival for patients with isolated pulmonary
metastases from PDAC undergoing pulmonary resections with low morbidity and mortality. This study