Page 451 - Read Online
P. 451
Li et al. Hepatoma Res 2020;6:39 I http://dx.doi.org/10.20517/2394-5079.2020.13 Page 3 of 7
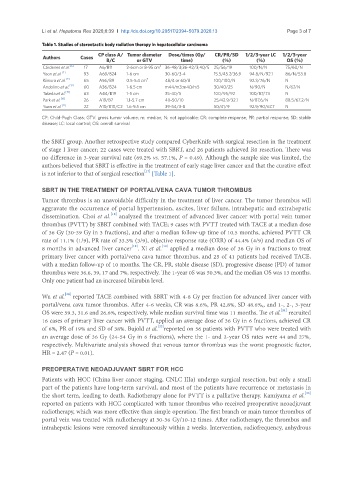
Table 1. Studies of stereotactic body radiation therapy in hepatocellular carcinoma
CP class A/ Tumor diameter Dose/times (Gy/ CR/PR/SD 1/2/3-year LC 1/2/3-year
Authors Cases B/C or GTV time) (%) (%) OS (%)
Cárdenes et al. [6] 17 A6/B11 2-6cm or 8-95 cm 3 36-48/3;36-42/3;40/5 25/56/19 100/N/N 75/60/N
Yoon et al. [7] 93 A69/B24 1-6 cm 30-60/3-4 15.5/45.7/36.9 94.8/N/92.1 86/N/53.8
Kimura et al. [9] 65 A56/B9 0.5-5.4 cm 3 48/4 or 60/8 100/100/N 92.3/76/N N
Andolino et al. [12] 60 A36/B24 1-6.5 cm m44/m3;m40/m5 30/40/25 N/90/N N/67/N
Takeda et al. [13] 63 A44/B19 1-5 cm 35-40/5 100/95/92 100/87/73 N
Park et al. [16] 26 A19/B7 1.1-5.7 cm 40-50/10 25/42.9/32.1 N/87.6/N 88.5/67.2/N
Yuan et al. [17] 22 A10/B10/C2 1.6-9.5 cm 39-54/3-8 50/41/9 92.9/90/67.7 N
CP: Child-Pugh Class; GTV: gross tumor volume; m: median; N: not applicable; CR: complete response; PR: partial response; SD: stable
disease; LC: local control; OS: overall survival
the SBRT group. Another retrospective study compared CyberKnife with surgical resection in the treatment
of stage I liver cancer; 22 cases were treated with SBRT, and 26 patients achieved R0 resection. There was
no difference in 3-year survival rate (69.2% vs. 57.1%, P = 0.49). Although the sample size was limited, the
authors believed that SBRT is effective in the treatment of early stage liver cancer and that the curative effect
is not inferior to that of surgical resection [Table 1].
[17]
SBRT IN THE TREATMENT OF PORTAL/VENA CAVA TUMOR THROMBUS
Tumor thrombus is an unavoidable difficulty in the treatment of liver cancer. The tumor thrombus will
aggravate the occurrence of portal hypertension, ascites, liver failure, intrahepatic and extrahepatic
dissemination. Choi et al. analyzed the treatment of advanced liver cancer with portal vein tumor
[18]
thrombus (PVTT) by SBRT combined with TACE; 9 cases with PVTT treated with TACE at a median dose
of 36 Gy (30-39 Gy in 3 fractions), and after a median follow-up time of 10.5 months, achieved PVTT CR
rate of 11.1% (1/9), PR rate of 33.3% (3/9), objective response rate (ORR) of 44.4% (4/9) and median OS of
[18]
8 months in advanced liver cancer . Xi et al. applied a median dose of 36 Gy in 6 fractions to treat
[19]
primary liver cancer with portal/vena cava tumor thrombus, and 25 of 41 patients had received TACE,
with a median follow-up of 10 months. The CR, PR, stable disease (SD), progressive disease (PD) of tumor
thrombus were 36.6, 39, 17 and 7%, respectively. The 1-year 0S was 50.3%, and the median OS was 13 months.
Only one patient had an increased bilirubin level.
Wu et al. reported TACE combined with SBRT with 4-8 Gy per fraction for advanced liver cancer with
[20]
portal/vena cava tumor thrombus. After 4-6 weeks, CR was 8.6%, PR 42.8%, SD 48.6%,, and 1-, 2-, 3-year
OS were 59.3, 31.6 and 26.6%, respectively, while median survival time was 11 months. Tse et al. recruited
[21]
16 cases of primary liver cancer with PVTT, applied an average dose of 36 Gy in 6 fractions, achieved CR
[22]
of 6%, PR of 19% and SD of 38%. Bujold et al. reported on 56 patients with PVTT who were treated with
an average dose of 36 Gy (24-54 Gy in 6 fractions), where the 1- and 2-year OS rates were 44 and 27%,
respectively. Multivariate analysis showed that venous tumor thrombus was the worst prognostic factor,
HR = 2.47 (P = 0.01).
PREOPERATIVE NEOADJUVANT SBRT FOR HCC
Patients with HCC (China liver cancer staging, CNLC IIIa) undergo surgical resection, but only a small
part of the patients have long-term survival, and most of the patients have recurrence or metastasis in
[23]
the short term, leading to death. Radiotherapy alone for PVTT is a palliative therapy. Kamiyama et al.
reported on patients with HCC complicated with tumor thrombus who received preoperative neoadjuvant
radiotherapy, which was more effective than simple operation. The first branch or main tumor thrombus of
portal vein was treated with radiotherapy at 30-36 Gy/10-12 times. After radiotherapy, the thrombus and
intrahepatic lesions were removed simultaneously within 2 weeks. Intervention, radiofrequency, anhydrous